Sex crime DNA destroyed, rape victims ignored
Vital DNA evidence from sex crimes had been “accidentally destroyed” and rape victims were forced to wait up to 12 hours before having a forensic exam, an inquiry has heard.
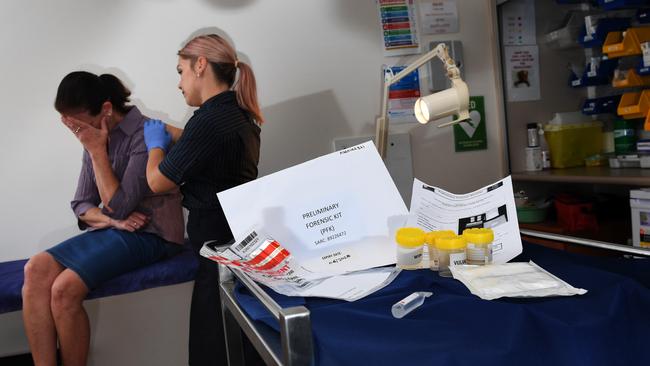
Vital DNA evidence from sex crimes had been “accidentally destroyed” and rape victims were forced to wait up to 12 hours in the clothes in which they were assaulted before having a forensic examination, a women’s safety inquiry has heard.
A 16-month review, led by former Court of Appeal president Margaret McMurdo, has delivered a scathing assessment of the way Queensland Health delivers forensic services and recommended more doctors and nurses be hired and trained to ensure statewide access to care.
Sexual assault victims, including children, have been turned away from regional hospitals because there were no medical staff available to conduct forensic medical exams, also known as rape kits, and large hospitals have kept patients waiting for up to 12 hours.
Many victims are required to sit for hours in cold, isolated rooms, with no food, water or clean clothing.
A 16-year-old rape victim was told by hospital staff in north Queensland that they were too busy to see her; they asked her to return 36 hours later for an examination, the Cairns Sexual Assault Service told the inquiry.
The teenager was also asked not to shower in the interim. It was not until police advocated for her that the hospital agreed to do the examination, some eight hours later.
Another victim spent nine hours at a Brisbane hospital in the clothes in which she was attacked, and was asked not to urinate in case it impacted evidence.
Gold Coast Forensic Medical Unit deputy director Cathy Lincoln told the inquiry there were simply not enough trained forensic medical physicians in Queensland.
The McMurdo inquiry recommended that all doctors and emergency nurses be trained to provide forensic medical examinations and “clearly understand that this is a significant part of their role”.
“The taskforce notes the advice received from Queensland Health about difficulties in recruiting emergency doctors in a tight labour market (and) also notes the concern that making forensic examination a fixed requirement of emergency doctors’ employment may deter doctors from working in Queensland,” it said.
Queensland Health confirmed it has already begun an international campaign to recruit overseas nurses and was in the early stages of a drive to entice health workers from interstate.
The inquiry also heard of disturbing problems with evidence collection and storage.
One rape victim told the inquiry that about a month after the invasive swab tests were collected during her forensic exam, she was phoned and told “the police had accidentally destroyed the rape kit/DNA evidence and they were ‘very sorry’. This meant the case had no real chance of proceeding,” she told the inquiry.
Another victim described a “category of errors” in her case that included “losing clothing worn during the attack, taking invasive forensic evidence and not testing it, and charging the wrong perpetrator”.
“Only one was charged … based on DNA evidence despite there being three rapists,” she said.
“The officer who lost the evidence and mishandled the case was fined.”
In a statement, Queensland Health acknowledged findings from the taskforce and said it was “carefully considering” them.
“We understand the importance of reviewing our policies to ensure the services we deliver to any person, at any hospital, remain suitable and supportive.
“We have implemented reforms aimed at providing more support for victims who present at our hospitals. This includes investing $1.39m to increase training in forensic procedures in all public hospitals.”








To join the conversation, please log in. Don't have an account? Register
Join the conversation, you are commenting as Logout