This was published 4 years ago
Opinion
How will variants change our response to COVID-19?
By Brendan Crabb and Mike Toole
The growing outbreak of COVID-19 in Sydney’s suburbs has cast a spotlight on the Delta variant of the SARS-CoV-2 virus. We are now on day 28 of the outbreak and already 864 cases have been reported, whereas during Victoria’s second wave this number was not reached until Day 38.
This is despite NSW having better public health systems and control measures in place than Victoria did a year ago. This sums up the impact and seriousness of the increased infectiousness of Delta compared with the original Wuhan strain. So what are the broader implications of the emergence of this variant and future variants and how will it change the way Australia – and the world – contains the pandemic?
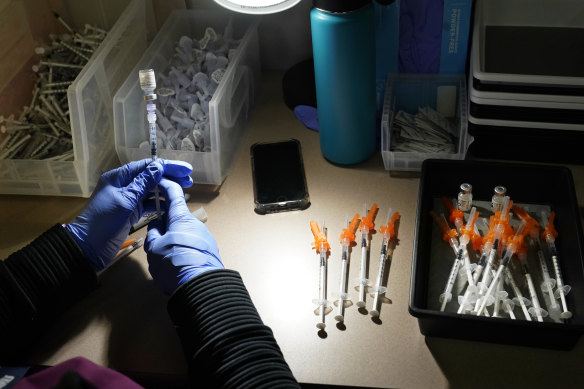
A nurse fills syringes with Pfizer vaccines at a COVID-19 vaccination clinic. Credit: AP
What is a variant?
All viruses change over time, especially viruses that have a genome made of RNA rather than DNA. RNA genomes are often not copied as faithfully as DNA genomes, meaning as the virus replicates its genes undergo random “copying errors” (ie. genetic mutations). Over time, these errors can lead to alterations in various viral proteins. The process of natural selection then comes in to play, if the “mutant” virus has a survival advantage then it will outcompete its parent and before long this mutant, or “new variant”, will be the dominant virus detected.
Apart from coronaviruses, influenza viruses are a well-studied example of an RNA virus that mutates frequently, in fact more frequently than coronaviruses. In fact, much of our knowledge of how viruses change comes from observing the influenza virus. The influenza virus mutates so often that each year a new vaccine has to be developed to provide protection against seasonal flu. From what has been observed so far of SARS-CoV-2, it appears that the virus is mutating about four times slower than influenza.
Most mutations do not give the coronavirus any advantages over earlier strains and simply reach a dead end. However, some mutations on the surface spike protein have allowed the virus to enter the body’s cells more easily and, therefore, be more infectious. Other mutations allow the virus to avoid (usually partially) the immune response mounted through natural infection or vaccines.
The World Health Organisation has designated four variants of concern and a number of variants of interest. The four variants of concern, which emerged in 2020, are Alpha, first detected in England, Beta (South Africa), Gamma (Brazil) and Delta (India). These variants have been proven to effect infectiousness, severity of illness and immunity conferred by previous infection and vaccines to different degrees.
Why is Delta so worrying?
First reported in the Indian state of Maharashtra, Delta quickly became the dominant strain across India and has spread to about 98 nations, including the UK, southern Africa, Myanmar, Fiji, Vietnam and Singapore. It has caused community outbreaks in Sydney, Melbourne, Darwin and Perth.
In just two months, Delta replaced Alpha as the dominant strain of SARS-CoV-2 in the UK. The increase is primarily in younger age groups, a large proportion unvaccinated. WHO estimates that the variant is 55 per cent more transmissible than the Alpha variant, which was in turn around 50 per cent more transmissible than the Wuhan strain. That means someone infected with Delta can infect up to six or seven others compared with two to three others with the Wuhan strain. That can quickly lead to exponential spread.
The top five symptoms of the Delta variant are headache, sore throat, runny nose, fever and cough.
The good news is that the mainstay vaccines still offer good protection but it is reduced. A study in England found that one dose of AstraZeneca or Pfizer is only 33 per cent protective against symptomatic COVID-19 caused by Delta, a significant drop from the protection against the original strain. However, a Scottish study found that two doses of Pfizer and AstraZeneca provide 79 per cent and 60 per cent protection, respectively, and the protection offered against severe disease remains exceptionally high.
According to a UK study, the initial symptoms associated with the Delta strain are different from those experienced in 2020. The top five symptoms are headache, sore throat, runny nose, fever and cough. Loss of smell comes in at number 9 and shortness of breath comes far down the list at number 30.
What should we do differently to contain Delta?
Compared with this time last year, we now have two important advantages: a range of safe and effective vaccines and a greater understanding of how the virus spreads and how it can be contained. Most of the world is not yet adequately vaccinated to prevent further outbreaks and that includes Australia. An accelerated global rollout of vaccines is the best way to emerge from the pandemic; however, it is almost inevitable that booster shots will be necessary in the coming year. Meanwhile, there are additional measures that will help us navigate through inevitable outbreaks.
As soon as a cluster of community transmission emerges, with doubling of daily cases, the early imposition of masks and strict physical distancing measures has been proven to quickly bring outbreaks under control and prevent prolonged lockdowns. This is even more essential to contain the more infectious Delta variant.
Because Delta spreads so rapidly it is important to quickly identify close contacts and their contacts to ensure they test and isolate.
Communications with the public to encourage testing need to point out the change in common symptoms that now resemble winter colds. Because Delta spreads so rapidly it is important to quickly identify close contacts and their contacts to ensure they test and isolate.
It is more crucial than ever that attention be given to indoor ventilation to prevent airborne transmission, especially in healthcare settings and quarantine hotels. All frontline workers need to be fully vaccinated and have access to effective respiratory masks.
The rapid dominance of the Delta variant across the world poses one of the greatest challenges during the entire pandemic. And it’s a huge warning shot. As long as the pandemic is allowed to run anywhere in the world, newer and even more concerning variants will emerge. A comprehensive “Vaccine Plus” strategy, rigorously implemented throughout the entire world, is the only option to chart a course through this difficult period.
Professor Brendan Crabb is a microbiologist and director of the Burnet Institute and Professor Mike Toole is an epidemiologist and technical adviser to the Know-C19 Knowledge Hub at the Burnet Institute.