This was published 3 years ago
How did Australia’s vaccine rollout turn into a ‘train wreck’?
Promises not delivered; doses announced, reannounced and still there are not enough. Vaccination has turned into a political problem for the federal government. This is how it went wrong.
By Farrah Tomazin and Clay Lucas

Dr Michael Clements in Townsville, who recently had to throw away unused AstraZeneca vaccines for lack of interest.
Four months after Australia’s COVID-19 vaccination program began, Michael Clements paced the halls of a medical clinic in north Queensland, trying to recruit patients willing to be inoculated with AstraZeneca.
It was late June and the Townsville-based doctor was visiting the outback town of Julia Creek to help the local GP and see how vaccinations were tracking. He found a fridge filled with unused vials. A lack of demand from patients meant the batches were about to expire.
“I was literally walking the halls to see if anybody wanted it,” Clements says.
“The federal government at that stage had been telling people ‘Well if you just wait, you can get the vaccine of your choice’, so people were just waiting until they could get Pfizer. We were throwing out vials and vials of the vaccines.”
“We’ve got hundreds of doses that we know are about to expire soon, and we just can’t find anybody to take it.”
Eighteen months after Australia’s first case of coronavirus was reported in Victoria and seven months since the Pfizer jab became the first vaccine approved for the country, Australia’s national vaccination program continues to be confusing at best, and a shambles at worst.
Many people cannot access the vaccine they prefer, while a perfectly effective jab is being tipped down the sink. Australia has inoculated the third-lowest proportion of its population of any OECD nation, with only 18 per cent of over-16s fully vaccinated.
Meanwhile hundreds of millions of dollars have gone to consulting firms for advice that remains shrouded in secrecy, and to ad agencies for campaigns that have either run before vaccines were available or have been a flop.
And there have been many missed targets. Prime Minister Scott Morrison, who once insisted the vaccine rollout was “not a race,” now concedes the program is at least two months behind schedule.
What went wrong is a mixture of bad luck, politics, poor procurement decisions and mixed messages about the safety of one of the rollout’s key vaccines: AstraZeneca. According to Grattan Institute health program director Stephen Duckett, Australia’s vaccine strategy has been among “the worst in the world”.
“Shitstorm is the word of the moment,” he says.
‘Top of the queue’
In January last year, nine days after China confirmed the sequence of COVID-19, University of Queensland professor Paul Young received an email that would galvanise his team. For months, scientists at the university had been working on an exciting new technology. Called a “molecular clamp”, it promised to make vaccine development faster and more agile.
On January 21, 2020, an official from the global vaccine-development body, the Coalition for Epidemic Preparedness Innovations, emailed the university to ask if their invention might be used to create a new COVID vaccine.
Young’s team took up the challenge and produced a vaccine candidate. The Morrison government ordered up big, taking an initial 51 million doses.
This untried technology would form half the initial backbone of Australia’s entire vaccine strategy. The other half involved AstraZeneca, based on a more traditional technology, much of which was to be produced in Melbourne by biotech firm CSL.

Paul Young: the University of Queensland’s molecular clamp technology had some difficulties.Credit: Michelle Smith
Stung by criticism over the early unavailability of personal protective equipment and even hand sanitiser due to our reliance on suddenly shaky international supply chains, the federal government was desperate to have its vaccine supplies manufactured on home soil.
According to Morrison at the time, the UQ candidate and AstraZeneca would put Australia “at the top of the queue if our medical experts give the vaccines the green light”. But both failed to pay off as planned.
AstraZeneca ran into reputational issues with the very rare risk of a blood-clotting side-effect. The UQ vaccine did not make it past phase one trials, where it turned up some false positive HIV results, mainly because the vaccine’s signature “clamp” technology contained an HIV protein.
“We were devastated,” Young says now of the government’s decision to dump the UQ project last December. “We argued at the time that there may be some value in going forward to phase two and three of our trials and then making a decision, but the window of opportunity to progress wasn’t taken.”
Other countries, meanwhile, pushed ahead.
A disputed meeting
On a hot July afternoon in Washington, DC, four months before last year’s US presidential election, Donald Trump stood at the lectern in the James Brady briefing room of the White House and announced a new deal to secure the nation’s supply of coronavirus vaccines.

Donald Trump in July 2020 spruiking the vaccine candidates.Credit: Bloomberg
Under the agreement – now one of six secured by the US with various manufacturers – the government would pay $1.95 billion for Pfizer to produce and deliver 100 million doses of a vaccine once it was approved by America’s drug regulator. Another 500 million doses would be delivered shortly afterward through the Trump administration’s aptly titled procurement strategy, Operation Warp Speed.
“This is another crucial step in our effort to develop, manufacture and distribute a vaccine in record-breaking time,” Trump declared.
On the other side of the globe, in Australia, things were not moving so fast.
Twelve days before Trump’s “historic announcement”, Pfizer had met with the Morrison government. The US pharmaceutical giant, which had partnered with German firm BioNTech to deliver the Comirnaty vaccine, had written to the government two weeks earlier requesting a meeting.
When the company and officials from the Department of Health sat down, according to the government’s Lisa Schofield, assistant secretary of Canberra’s vaccine taskforce, Pfizer presented “a preliminary view of where they were up to and what they were thinking”.
“We were interested in talking to them about potentially purchasing that vaccine, but that was it,” Schofield told a Senate hearing in June. “No numbers or details were put on the table.”

ABC’s Norman Swan stands by his reporting that the government botched a Pfizer deal in July 2020, which was based on anonymous sources but denied by those in the meeting. Credit: Janie Barrett/Meredith O’Shea
Others have presented a different view. According to ABC Coronacast host Norman Swan, three unnamed sources told him that Pfizer had wanted to use Australia as a global example for its vaccine rollout, but in that July meeting a Department of Health representative had demanded access to the company’s intellectual property and haggled over the cost.
The government and Schofield have denied that version of events.
Whatever the truth, the US, Canada, Japan and Britain all struck agreements with Pfizer in July and August 2020. It wasn’t until November last year that Pfizer signed contracts to supply 10 million doses to Australia in 2021 – enough to fully vaccinate only five million people. They were meant to be rolled out in the first three months of the year.
The first doses of Pfizer arrived on February 15, with Prime Minister Scott Morrison receiving his first jab on February 21 alongside an aged care resident. That same month the company agreed to supply 10 million more doses in mid-2021. Then in April the order was doubled again, meaning in the final quarter of this year 20 million more Pfizer doses will arrive on Australian shores.
Duckett believes the government’s procurement decisions at a time when other countries were investing heavily in a broader range of vaccines paved the way for the slow response to the pandemic.
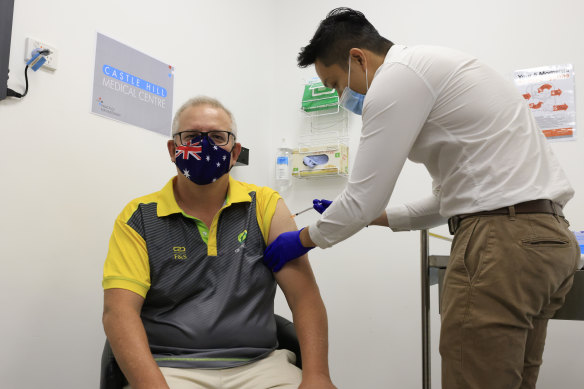
Prime Minister Scott Morrison gets his Pfizer jab in February.Credit: Getty
But other decisions taken early have also contributed to the slow rollout. The Commonwealth kept a tight rein on the process and initially limited the role of the states. Doses went to the wrong places. There was confusion around aged care centres, where contractors offered vaccines to residents but left the vast majority of staff unvaccinated. Since then, staff vaccinations has been made compulsory, but by this week only 28 per cent of staff had been fully vaccinated, while 48 per cent had had their first shot. Of 186,00 residents living in 2600 aged care homes that the Commonwealth is responsible for, 83 per cent are now fully vaccinated, and all have been offered a vaccination. But even that rollout came months late.
“It’s been a trainwreck,” says Duckett, a former federal health department secretary, “a complete shemozzle”.
University of Sydney immunisation researcher Julie Leask is more sympathetic, believing Australia will eventually achieve high COVID-19 vaccine coverage, even if the rollout has been slow and problematic.
“Our expectations were sky-high and to some degree unrealistic because new vaccine rollouts are always complex,” she says. “It certainly has been mired in federal government failures. But it’s been a problem of supply – we don’t have enough Pfizer – combined with the safety issue around the use of AstraZeneca vaccine.”
Limboland
These factors have helped create a perfect storm for the latest wave of COVID-19. Australia is now in a period of limbo, with the highly contagious Delta variant resisting contact tracing and the lingering threat of further lockdowns until more people are inoculated. On Friday, Morrison announced more details of a four-stage plan. We will be in a supression phase - fast lockdowns - until we reach 70 per cent fully vaccinated, and 80 per cent vaccinated before we begin to treat COVID-19 as an illness to manage, rather than suppress. We are months away from those targets.
Last week, as NSW declared a “national emergency” after community transmission continued to soar despite a month in lockdown, Premier Gladys Berejiklian urged other states to divert their allocations to help NSW drive down COVID cases. Faced with outbreaks of their own, Victoria and South Australia declined. Morrison supported their decision.
Few were surprised by the reluctance of the states to share their doses with NSW. After all, the impact of the Commonwealth’s decision not to order enough Pfizer vaccines had already hit home in Victoria when the state had been forced to halt the number of people getting their first doses of the drug to ensure there was enough supply for people who needed their second jab.
By that stage, Victoria had been plunged into its fourth lockdown in 15 months, but had only been getting a weekly allocation of 71,370 doses of Pfizer. It was a turning point in state-federal relations: the limited supply meant that when eligibility for vaccine was extended to 40 to 49-year-olds, many people were unable to make phone bookings for their first dose and those who walked up to mass vaccination hubs were turned away. It wasn’t until June 14 – the day the state announced a pause in first doses – that a further 105,300 doses were allocated by the Commonwealth.
As Victorian Deputy Premier James Merlino would later put it: “The 800-pound gorilla in the room that we have failed to mention today is the fact that we’re in this position because our vaccination program has not delivered what we were told it was going to deliver.”
A clot in the system
Two weeks ago Andrew McLeod and his wife Julie sat in a COVID mobile clinic in tropical north Queensland where they had just received their second jab of Pfizer.
The couple, both aged in their mid-60s, had the option of taking AstraZeneca but chose not to – partly because of what they’d read in the media about the rare risks involved, and partly because their own GP had advised them against it.
“My wife is a chronic asthmatic and so I spoke to my doctor to ask what we should do,” he tells The Age and The Sydney Morning Herald. “She’s a great doctor – 36 years old and a real gem – and she basically told us: ‘If I were you, I’d hang out for the Pfizer’.”
They’re not alone. The latest figures from the Bureau of Statistics show that one-third of people aged 50 to 69, and a quarter of people aged 70 and over – who have been eligible to get vaccinated since March – were not getting jabbed because they are waiting for a different vaccine.
Part of the problem has been the changing advice on AstraZeneca by the Australian Technical Advisory Group on Immunisation (ATAGI), which makes recommendations to the government on how the vaccines should be administered.
On April 8, ATAGI lowered the preferred age for AstraZeneca shots and recommended Pfizer as the vaccine of choice for under-50s (the advice on AstraZeneca followed Britain’s lead; the UK later revised its guidelines so anyone over 40 was believed safe to get AstraZeneca).
On June 17, the age threshold changed again, in part due to global nervousness, this time to under-60s. And by June 28, there was another shift, when Morrison made a surprise announcement and suggested that Australians under 40 should speak to their GP about getting the AstraZeneca jab, contradicting ATAGI’s earlier advice.
This led to Queensland’s chief health officer rebuking Morrison’s intervention, bluntly declaring: “I do not want under-40s to get AstraZeneca. It is rare, but they are at increased risk of getting the rare clotting syndrome.”

Queensland Chief Health Officer Jeannette Young took on Scott Morrison and AstraZeneca.Credit: Getty
The confusion has fuelled vaccine hesitancy, despite the overwhelming safety of the drug, which has been enthusiastically used around the globe. Indeed, this week, as NSW’s outbreak continued to worsen, ATAGI revised its advice yet again, stating that anyone over the age of 18 in greater Sydney should consider getting the drug, while Morrison practically pleaded with Australians to increase their take-up.
“The Pfizer doses, of course, are increasing, but the AstraZeneca is there – and that gets us to our goal a lot faster,” he said.
Australians’ willingness to close borders, lock down and follow the rules have led to low rates of COVID-19, but have arguably also resulted in vaccine complacency.
“It’s very important to put into perspective here that our death rate is virtually unmatched by anybody other than New Zealand and a few other countries,” Health Minister Greg Hunt told The Age. Sydney University last week published a study showing lockdowns – predominantly led by the state governments – have saved 48,000 lives.
The Commonwealth denies it failed to build up a broad portfolio of vaccines, saying it has secured five agreements that together provide 195 million doses. On top of the Pfizer deal for 40 million doses and AstraZeneca, backing them up are the Moderna and Novavax vaccines (Novavax trials have shown it is very effective, but it is not yet approved for use anywhere in the world). Half a million Moderna doses will be available per week from October. It means the government’s suite of vaccines will be more than enough to cover the whole adult population. And from August, almost 4000 pharmacists will join GPs in providing jabs, starting firstly with AstraZeneca.
Nonetheless, Hunt is under intense pressure with some – including former PM Kevin Rudd – having called for him to resign and laying the blame directly at the feet of the Morrison government.
“We’ve got a fully blown national emergency on our hands because Scott Morrison failed to secure enough vaccines to protect the Australian people,” says Labor’s opposition spokesman Mark Butler. “World’s best practice is to have four to six vaccine deals – Labor was calling on the Government to do this last year.”
Hunt defends the program and turns any discussion about past failures to focus on where we are now. He is particularly belligerent about Norman Swan’s accusations his health department turned away Pfizer in mid-2020, describing this as “false”.
“People say ‘Why didn’t you spend more on Pfizer?” But there was no more available,” says Hunt, with mass deaths across Europe and North America and producers in those countries focused on their own sick citizens.
“The US and Europe were prioritising themselves – and I don’t mean that critically,” says Hunt. “The company said to us, ‘Our doses in Australia will help you but they will save lives as soon as they are put into arms in Europe and North America’.”
Here come the consultants
The lack of vaccines might be a defining feature of Australia’s vaccine strategy, but it is not the only concern.
An Age and Herald analysis of government tender documents reveal that since last June, hundreds of millions of dollars have been spent on COVID-related contracts, with big consulting firms and ad agencies making many millions from the rollout. Yet much of their work remains shrouded in secrecy.
Accenture was awarded $7.3 million to develop a software solution to track and monitor vaccine doses, but the full extent of its data or the true costs involved has not been released, despite growing calls for a breakdown of vaccination rates across Australian suburbs and towns.
“We had hoped to have higher overall levels of vaccination … but the rates we’re achieving on a weekly and daily basis are certainly the marks we had hoped to be hitting.”
Prime Minister Scott Morrison
The Australian arm of McKinsey and Co was paid $2.2 million in March to give advice on how to manufacture mRNA vaccine – the same technology used to create the Pfizer jab. However the Industry Department declined to make McKinsey’s work public, citing commercial sensitivity. Similarly, the Health Department declined a request to release $1.8 million worth of research the bureaucracy paid to Sydney company FiftyFive5 into public sentiment towards vaccinations.
And more than $33 million was also spent on five advertising contracts in a year – most of which was paid months before Australians were able to be vaccinated when the rollout formally began in March.
Yet questions linger about the benefits of the ads. In the UK celebrities such as Elton John, actor Elizabeth Hurley and comedian Lenny Henry joined forces with the nation’s health service to encourage more people to get vaccinated, while in the US, ads featured former presidents Barack Obama, George W Bush and Bill Clinton getting the jab.
Australia’s public relations efforts – including an ad featuring former deputy chief medical officer Nick Coatsworth and an awareness campaign calling on people to “arm yourself” against COVID19 – have been viewed as lacklustre in comparison. There has been some feeling within the government that, without enough supply, it’s not really worth advertising.

Dr Nick Coatsworth from the government’s COVID-19 ad campaign.
And then there’s the mixed messaging about vaccine safety, fuelled in part by ATAGI, but also by sensationalist media coverage and social media.
Allen Cheng, the softly-spoken professor who recently stepped down from his role as Victoria’s deputy chief health officer, admits that the messaging has been “difficult” for the advisory group, which has “very carefully tried to craft the wording that we use” – but this has often been lost in translation.
“The best example of that is when we talk about the threshold for 50: we were very careful to use the term ‘We prefer people to get Pfizer’ and added that people should have autonomy and make up their own mind,” explains Cheng, who sits in the advisory group alongside experts such as Associate Professor Nigel Crawford, the head of Immunisation at the Royal Children’s Hospital, and Infectious Diseases Physician Professor Michelle Giles.
“The problem is people might read three lines of a newspaper story or hear us on the news and it doesn’t quite capture the nuance or tone.”
We don’t set targets ...
While the road out of COVID continues to be slow, Cheng says the vaccination program is gradually scaling up “and with increasing supply, hopefully a lot of the problems will start to go away”.
Scott Morrison is also optimistic. Asked if he stood by his new target to have every eligible Australian vaccinated by the end of the year, the PM replied: “That absolutely remains our goal by the end of the year, and we have the supplies to achieve that.
“We had hoped to have higher overall levels of vaccination … but the vaccination rates we’re achieving on a weekly and daily basis are certainly the marks we had hoped to be hitting by about this time of the year.”
The latest federal figures suggest almost 12 million doses have been administered, with 3.65 million Australians receiving their second jab. On July 1, just 8 per cent of Australians aged over 16 had received two doses of a vaccine; by Thursday this week, it had risen to 18 per cent.
The government is also considering how to manufacture mRNA in Australia – the cutting-edge technology used for Pfizer and Moderna vaccines, both of which need to be imported from overseas. However experts say this could take between one to three years and would require considerable funding.
Back in Brisbane, Professor Paul Young is optimistic. Seven months after the Morrison Government abandoned the University of Queensland’s vaccination trial, researchers are working on a “2.0” version of their clamp technology after data trials confirmed the first version, despite the false positive HIV results, was indeed safe – and potentially effective.
While the new vaccine is a long way off, he hopes it will play a role in fighting COVID19 in years to come, when the disease is embedded in the community, much like influenza.
But there’s a broader opportunity for the country too, Young says, as the vaccine rollout has exposed a glaring gap in Australia’s domestic manufacturing capability.
“The great irony in Australia is we have an amazing wealth of expertise in infectious disease research, but science isn’t translated as well or as rapidly as it could be, because we don’t have the infrastructure within the country to do that,” he says.
“On the back of this pandemic we could actually establish a new biomedical industry. It’s a fantastic opportunity – we just need investment.”