- Exclusive
- National
- Victoria
- Victorian budget
This was published 1 year ago
‘Have we learned nothing?’ Fears for pandemic preparedness as public health funding slashed
The Andrews government has slashed future funding for one of its most significant pandemic-era reforms: the local public health units established at the height of the COVID-19 crisis to rebuild the state’s public health capacity and defence against infectious disease.
Despite Health Minister Mary Anne-Thomas announcing a $103 million funding “boost” to support the work of the nascent local units, last month’s state budget concealed deep cuts that will reduce funding for the nine metropolitan and regional units by 40 per cent over the next two years.

A contact tracing team at the South Eastern Public Health Unit in 2021, set up to track COVID-19 outbreaks.Credit: Justin McManus
Government funding for the units will shrink from about $80 million this financial year to $55 million in 2023-24 and further reduce to $47 million in 2024-25. On July 1, as Victoria enters its peak season for flu and other respiratory viruses, dozens of public health officers will be out of a job.
This comes as local public health units take on more responsibility for managing outbreaks of communicable disease across the state.
The Public Health Association of Australia said the funding decision was short-sighted and disappointing, while senior figures within Victoria’s Department of Health, speaking anonymously to discuss budget matters, said it sent a terrible message about the importance of public and preventative health.
“This is just the wrong direction in terms of investing in public health in Victoria,” said the association’s chief executive, Terry Slevin. “I would have thought that Victorians, with the experience they had during the last pandemic, want to be not the worst prepared in the world but the best prepared in the world for when we go around again.”
In response to questions provided by this masthead, a Department of Health spokesperson said the funding cut reflected the end of “temporary surge funding for the COVID-19 response” and that funding for other health prevention and promotion work done by the local units was unchanged.
“The change reflects the reduced impact COVID-19 is now having and that the response to COVID is now more aligned with other communicable diseases,” the spokesperson said.
A government spokesperson said the $103 million figure cited by Thomas was for the combined two years of funding for local public health units. “Previously our [local units] were funded year to year, and the two-year funding certainty will give them the ability to invest in long-term responses to the public health challenges faced by their communities,” he said.
Sources with knowledge of the local public health units said that although the budget cut was partly explained by the cessation of COVID-specific funding, its impact would be felt beyond COVID-related work.
The North Eastern Public Health Unit, one of three metropolitan local units and which services 1.7 million people including some of Melbourne’s most socio-economically disadvantaged communities, last week informed a third of its approximately 90 staff they would not have a job at the end of this month.
The Western Public Health Unit, which covers a massive patch stretching from Melbourne’s CBD to Sunbury in the north and Little River in the south-west, is also making substantial staff cuts to meet its post-pandemic budget.
The South East Public Health Unit has been less affected by the budget cuts due to an earlier decision by Monash Health to fund the local public health unit through its own budget and transfer staff from short-term contracts to ongoing positions. The Barwon SW, Grampians and Loddon Mallee units declined to comment on the impact of the budget cut on their staffing levels.
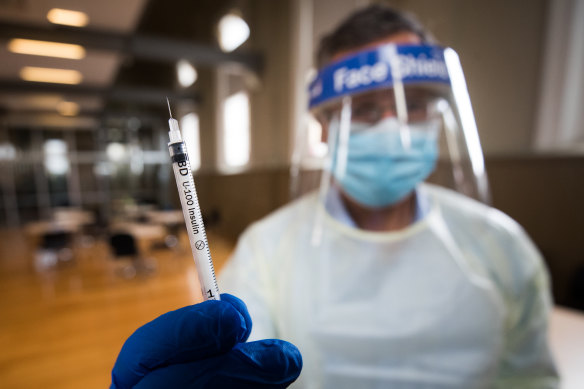
The Barwon South West Public Health Unit offered COVID-19 vaccine booster shots from 2021.Credit: Jason South
The local public health units were established in October 2020 when Victoria was in the depths of a second wave COVID-19 epidemic that forced the state into the first of two successive winter lockdowns.
The formation of the units, which the Andrews government modelled on the decentralised public health structures of NSW and Queensland, shifted pandemic response teams out of the heath department’s Lonsdale Street headquarters and into local hospital networks. The change contributed to Victoria’s improved management of COVID-19 outbreaks in 2021.
The health minister who oversaw the introduction of the local units, Martin Foley, described them last year as an enduring reform that would help address socio-economic inequities in Victoria’s heath system.
“If you are rich and white and in the south-east and eastern suburbs, your chance of having got through this pandemic were a whole lot better than if you weren’t,” he told this masthead shortly before he resigned as health minister. “The capacity of local public health units to deal with those structural inequalities will be built considerably.”

Enduring reform: Former health minister Martin Foley oversaw the establishment of local public health units.Credit: The Age
Foley’s successor, Thomas, has set the local units an ambitious task. They will, by the end of this year, be responsible for managing outbreaks of all notifiable infectious diseases in Victoria other than tuberculosis.
This includes COVID-19, hepatitis, meningococcal and pneumococcal infections, some sexually transmitted infections, influenza and respiratory syncytial virus – a leading cause of infant hospitalisations.
Opposition health spokesperson Georgie Crozier said the funding cuts would deliver savings in the short term, but leave Victoria exposed.
“Have we learned nothing about the value of these units?” she said. “When you have outbreaks, you can’t manage this stuff from Lonsdale Street. It is the wrong time to be cutting the budgets of these programs.”
University of Melbourne professor Nathan Grills, a public health physician who oversees a government-funded public health training program, said continued investment was needed to develop the capacity of the local public health units and a stronger culture of public health.
“Under-investment by previous governments came to the fore during the pandemic and we paid a price for that,” he said. “Any decrease in investment in public health may be a short-term fix for the budget, but it won’t promote our health in Victoria long-term.”
Grills last week wrote to the health department seeking more training places for public health physicians. Victoria has fewer public health physicians per capita than any state or territory, according to the most recent figures published by the Australian Health Practitioner Regulation Agency.
At the start of the pandemic in January 2020, Victoria had a single, centrally located public health unit within the department called the health protection branch. It employed nine public health officers.
By comparison, NSW and Queensland each had a well-established network of public health units embedded in local hospitals and health services across their capital cities and regional areas.
The disparity prompted then health minister Jenny Mikakos to warn senior colleagues, shortly after Victoria recorded its first COVID-19 case, that the state’s frontline defence against communicable disease was in disrepair.
A senior health department figure, speaking on condition of anonymity because they were not unauthorised to publicly discuss the matter, expressed frustration at the prioritisation of acute health services over preventative and public health measures.
“All the attention is at the pointy end – triple zero calls, ambulance times, emergency department wait times, 24-hour stays and surgical wait lists,” they said.

Premier Daniel Andrews and Health Minister Mary-Anne Thomas speaking after the release of last month’s state budget.Credit: Wayne Taylor
In the lead-up to last year’s state election, the Public Health Association of Australia and the Australian Health Promotion Association called for total annual funding for the local public health units to be increased to $150 million – almost triple the 2023-24 allocation in last month’s budget.
Under the federal government’s National Preventive Health Strategy, released two years ago, 5 per cent of total Commonwealth and state government funding should be invested in public health by 2030.
The Public Health Association of Australia estimates that Victoria spends 2 per cent of its health budget on public health.
The Morning Edition newsletter is our guide to the day’s most important and interesting stories, analysis and insights. Sign up here.