This was published 2 years ago
Nearly 10,000 Australians have died from COVID-19. Who is still dying?
By Mary Ward and Melissa Cunningham
As new Omicron sub-variants drive rising infections and states observe steadily increasing hospitalisations, Australia will report its 10,000th death from COVID-19 early next week.
The figure is barely a fraction of death totals recorded in similar countries around the world – in Britain, 10,000 had died from the virus by April 2020, and the same figure was recorded within just two months this year – but in a country which locked down to keep its death toll low, the shift to daily double-digit death figures has been swift.
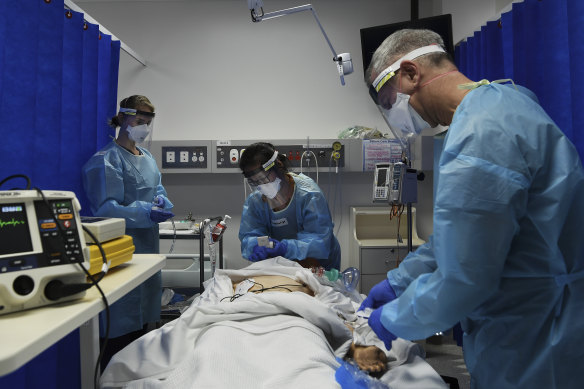
The number of reported COVID-19 deaths is likely to hit 10,000 next week.Credit: Kate Geraghty
So, in 2022, who is dying from COVID-19? Are health authorities concerned? And what can we do, if anything, to reduce their numbers?
The factor most likely to lead to death from COVID-19 is old age. About 40 per cent of deaths in NSW in the week ending June 25 were people in their 90s, and more than three-quarters were aged 80 and older.
NSW Chief Health Officer Kerry Chant said this was a “typical pattern” for infections, noting older people and people with underlying health conditions had always been considered an at-risk group.
“People who are elderly and with a lot of underlying health conditions don’t have a lot of physiological reserves,” she said.
President of the Australia and New Zealand Society for Geriatric Medicine Vasi Naganathan agreed.
“Everything we’ve known about COVID, pretty much from the beginning, has said this was going to happen,” he said. “I’m not being blase about it: this is why we have been concerned all along about COVID.”
In older people, the most severe symptoms from an Omicron infection are often not respiratory, instead it affects physical and cognitive function, causing delirium, for example, leading to an overall decline. “They don’t recover to what they were once before, and some of those people die,” Naganathan said.
Victorian geriatrician Associate Professor Michael Murray, who oversees a number of in-reach teams in residential aged care said he was “seeing a lot more COVID-related deaths than ICU [admissions] now”.
In the week ending June 25, just eight people were admitted to NSW ICUs with COVID-19. Melbourne’s Austin Hospital intensive care director Stephen Warrillow said its ICU ward, once full of people critically ill with coronavirus, was now only treating “one or two” COVID patients a day.
This disparity between deaths and ICU admissions is mostly due to high numbers of deaths in aged care, after the removal of strict lockdown restrictions.
Over 2021, just 13 per cent of deaths from COVID-19 in NSW were in aged care, but in 2022 they were about 40 per cent of the state’s 2900 deaths reported. Most aged care residents – more than four-fifths – die without being transferred to hospital.
Chant said this was because frail older people with underlying health conditions may not be “suitable” for highly involved intensive care treatment, and will do better managing their infection at the facility with antivirals.
“It’s about patient-centred care, and respecting their wishes,” she said.
Nationally, there were 1906 deaths from COVID-19 in aged care between January 1 and June 24, compared with 686 during 2020 and 231 in 2021.
Uptake of fourth doses in aged care has been slow – only about 65 per cent of eligible residents – although geriatricians are also concerned about first booster uptake and the hundreds of residents who have not received any vaccination.
Paul Sadler, the interim chief executive of the Aged and Community Care Providers Association, said the booster program was in progress and working well overall. While aged care workers must be vaccinated, with the easing of restrictions on facilities allowing visitors, aged care remains vulnerable to virus outbreaks.
“It’s vital the government urgently addresses the aged care workforce shortfall in order to help avoid staff shortages and interruptions in care,” he said.

About 40 per cent of NSW’s reported COVID deaths were in aged care homes.Credit: Fairfax
Naganathan dismissed the suggestion aged care residents dying from the virus were likely to have died from another bug within the same timeframe.
“The data continues to show the mortality of COVID-19 is higher than influenza,” he said.
Indeed, across the whole population, measures of “excess death” have shown above average levels of death this year.
The Australian Bureau of Statistics says there were 4732 more deaths than expected in the first two months of 2022. The Actuaries Institute has modelled that over the first quarter of the year, there were 5100 extra deaths (13 per cent above what was expected pre-pandemic), with around 60 per cent of those deaths from COVID-19.
Associate Professor David Muscatello, an infectious disease epidemiologist at UNSW who has modelled deaths for NSW Health, said these figures indicated COVID-19 was still directly and indirectly causing more deaths than we would anticipate, a phenomenon also seen during flu seasons.
“What we are going to see coming up this winter is the impact of both COVID and influenza causing excess mortality,” he said.
In her practice, Dr Charlotte Hespe, NSW and ACT chair of the Royal Australian College of GPs, is seeing infections in “vulnerable people who we protected really well over the last two years”.
“Now it is creeping in,” she said.
Warrillow said he was also seeing rising numbers of immunocompromised people, including organ recipients, seriously ill with the virus, despite taking all the right precautions, including having their boosters.
“I’ve certainly personally cared for a number of patients recently, who lead healthy, busy lives and that’s the success of their organ transplant, but they’ve been terribly unlucky,” he said.
Many of the dead would have benefited from up-to-date vaccinations. In NSW, all 104 people who died in the week ending June 25 were eligible for a booster shot, but only 69 per cent had received a third dose.
“We are seeing under-penetration [of vaccines] in some high-risk communities,” Murray said of the Victorian experience, expressing a need to increase uptake among culturally and linguistically diverse groups.
Unlike in previous waves of the virus, Australia now has a suite of treatments for COVID-19. While antivirals once had to be administered in hospital, the federal government has purchased 1.3 million doses of two COVID-19 oral antivirals.

Paxlovid was listed on the PBS in March, but antivirals need to be taken early to be most effective.Credit: Bloomberg
However, uptake of the drugs has been low. Data from the federal Department of Health to June 19 shows about 49,000 people have been prescribed Molnupiravir, sold as Lagevrio, since it was put on the PBS in March, while almost 7000 received scripts for Paxlovid.
“We’ve got the potential to do more,” said Chant. “There is a bit of confusion in the community as to who is eligible.”
While the antivirals are highly recommended for the unvaccinated, this is not a condition for prescription. But there are some limitations. For example, while aged care residents are automatically eligible, contraindications with other medications mean some cannot receive Paxlovid. The drug must also be administered within five days of symptom onset.
Chant and Hespe urged patients who were likely to need antivirals to make a plan with a GP, with Hepse noting they were more effective if administered on day one rather than day five.
Professor Greg Dore, an infectious diseases physician at St Vincent’s Hospital, said this time pressure showed the importance of an ongoing testing and isolating regime.
But, while the antivirals can save lives, Naganathan said it was important to remember antivirals were given on a “treat many to save one” basis, and ultimately a severe infection like COVID-19 would always lead to death in some vulnerable people.
With monthly coronavirus deaths now hovering at above 1200, Murray said this was greater than the worst Australian flu month.
“This is somebody’s mother, grandmother and somebody’s relative so of course it’s very distressing for the individual and their family,” he said.
“It is the price of us opening up, of people in the community not being careful enough about trying to prevent transmission, or not getting vaccinated or not getting their third or fourth dose, which, in my view, increases everybody’s risk.”
The Morning Edition newsletter is our guide to the day’s most important and interesting stories, analysis and insights. Sign up here.