Explainer
- Explainer
- Coronavirus pandemic
COVID 2.0? How is Delta rewriting the pandemic?
What is the Delta variant that has sent so many Australians into lockdown – and what does it mean for the pandemic?
It’s been called a game-changer by doctors, and a “guerilla fighter” and “long-jumping Gold medallist” by politicians; it has spread at the shops and at the footy among strangers, infecting families and friends – and friends of friends – before anyone knew something was wrong. The newly evolved Delta variant is rapidly taking over as the fittest form of the coronavirus worldwide, driving resurgences from India to the highly vaccinated Israel and the United States. This winter, it’s sent much of Australia into lockdown. But variants have emerged before, and even outbreaks of Delta have been stamped out. Crucially, vaccines still work against it. So why does this variant have scientists so worried and how is it rewriting our infection control playbook?
Does the rise of Delta mark a new phase for the pandemic? Artwork by Stephen Kiprillis.Credit:
What is the Delta variant and why is it so ‘fit’?
Viruses mutate as they spread. Most of these tiny changes don’t do anything at all, some might make a virus weaker. But others offer an advantage, such as binding better to the ACE2 proteins this coronavirus uses to hack into our cells, and so becoming more infectious; or changing shape a little to dodge the defensive antibodies made by our immune systems (and vaccines). Over time, viral lineages with these advantageous mutations will start to out-compete others – evolution on the microscopic scale.
Now, for the first time during a pandemic, scientists are tracking COVID’s viral family tree as it spreads around the world. When mutations emerge that seem to also be affecting patients, such as faster spread or nastier illness, they might be named as “variants of concern”, the CSIRO’s COVID-19 leader Professor Seshadri Vasan explains. Delta is one of the four such variants that emerged in late 2020: Alpha, first detected in England, Beta (South Africa), Gamma (Brazil) and Delta, which fuelled India’s devastating second wave.
Delta is at least 50 per cent more infectious than Alpha, and twice as infectious as the virus that first came out of Wuhan in late 2019. Each person who caught that original virus infected about two or three other people – for Alpha that “reproduction number” or R0 was four to five. Delta’s RO is five to eight (higher than smallpox but much lower than measles). It’s about on par with chickenpox, according to the Centres for Disease Control and Prevention (CDC) in the US, exceeding the common cold, seasonal flu and the first two dangerous coronaviruses to emerge in modern times: SARS and MERS. In just two months, Delta replaced Alpha as the dominant strain of COVID in the UK, and it has now spread to about 100 countries, including the US where it has also taken over.
There’s evidence emerging that it might be better at evading antibodies, too, and causing more severe disease. It’s been linked to a higher hospitalisation rate in Scotland, Canada and the UK, and there seems to be more young people falling seriously ill, including in NSW ICUs. But further study is underway and, in the case of more severe cases among the young, epidemiologist Michael Toole notes “that could be because more older people are now protected by vaccines”.
Delta has reshuffled the usual symptoms of COVID a little too, according to data out of the UK, with people mostly reporting headaches, sore throats and runny noses, then fevers and coughs. The once-common loss of smell comes in at number nine and shortness of breath is way down the list at number 30.
But the good news is that most of the vaccines still appear to hold up very well against the variant – provided you get your full two doses – and slash your chance of passing the virus onto others by about half too.
How is Delta shaping Australia’s latest outbreaks?
To get a sense of why Delta has health officials so nervous, consider the case of the Sydney removalists who brought Delta back into Melbourne on July 8. Normally, contact tracers say there might be “three rings” of an initial breach like this – the positive case, those they came into contact with and then those people’s own contacts.
But when officials rushed to “put out the embers” of this latest outbreak, they were finding positive cases further out again – not just among the removalist’s clients and then their neighbours in the apartment tower, but among those neighbours’ friends. And more people infected again among the families of those neighbours’ friends in just a few days, COVID-19 response commander Jeroen Weimar said. ”This is probably the fastest response we’ve ever seen to an outbreak that’s moving much more quickly than we’ve ever seen here in Victoria or, I suspect, anywhere else in Australia.”
In NSW, where the outbreak kicked off in June after an unvaccinated (and unmasked) limousine driver caught Delta from an international flight crew, cases have been climbing faster than at the start of Victoria’s deadly second wave last winter, Toole and Brendan Crabb note at the Burnet Institute. It’s fast become the state’s worst outbreak since the pandemic began. “I’m incredibly concerned,” NSW Chief Health Officer Kerry Chant said. “When we find a case in a family, we find that everyone in that household [already] has the disease.” The numbers of the very ill are also creeping up, with more than 10 per cent of those diagnosed in NSW requiring hospitalisation, and younger people in the ICU.
Deakin University chair of epidemiology Catherine Bennett says the stakes for contact tracers are much higher now that every case is more likely to pass on the virus. “If you miss even one case, even if they just have casual contact with someone, you can get more. In public health, we know there will be breaches, but the rules are generally strong enough to work anyway, but Delta is like fine sand, it finds the cracks.”
Dr Finn Romanes has been running contact tracing in Melbourne’s western suburbs since the virus spread south and told ABC Radio Melbourne that the period between new clusters emerging was also narrowing this time around, from roughly three days to two, as people became infectious faster. One silver lining to that? “The cases will show up faster too,” Bennett says. “People will likely get sick almost all at once [in a household] rather than over weeks, one after the other ... so it might mean you can have those shorter, circuit-breaker lockdowns and they’ll have real effect.” On July 15, Victorian Premier Daniel Andrews announced one such five-day lockdown (the state’s fifth since the pandemic started) in order to buy contact tracers time to get ahead of the virus before “it just explodes”.
Bennett says Victoria and NSW, which locked down 10 days after the outbreak began up north, have both responded well so far. “But NSW realised they’d missed an outbreak in Western Sydney,” she says. “Now, Victoria’s throwing everything at it. They have two [incursions] of the virus, the removalists and a family from Hume. If Victoria can’t get on top of this virus with a five-day lockdown then that’s absolutely a warning sign about the version of Delta that’s spreading here. Everywhere it’s landed it’s caused problems so far.”
Is contact tracing and other infection control changing too?
Former department of health secretary Stephen Duckett, now at the Grattan Institute, quips that he’s still “old enough to remember March last year when everyone was certain the virus could only spread in big droplets one or two metres”. That led to all kinds of “hygiene theatre” such as screens, most of which offered little protection because, as Duckett notes, the virus is more like smoke. Without strong ventilation, it builds up in the air. And now, with even more infectious variants such as Delta, the definition of “close contact” has dramatically narrowed again. At the start of the pandemic, 15 minutes of face-to-face conversation or two hours in an enclosed space with a case was said to put you at risk of catching the virus. Now even “fleeting contact” can be enough, 5-10 seconds according to Queensland Chief Health Officer Jeannette Young. Passing someone at the shops or sitting in the same restaurant after they have left.
Because of this airborne spread, hotel quarantine was overhauled to stop the virus ripping through floors (particularly in Melbourne, where it was the scene of the catastrophic leak that ignited last year’s second wave). “But we keep seeing breaches around the country, people opening doors at the same time as someone infected on their floor, because we still don’t have our open-air quarantine cabins,” Toole says. “We need them in every state, especially NSW – they get the most international travellers but they never talk about it.”
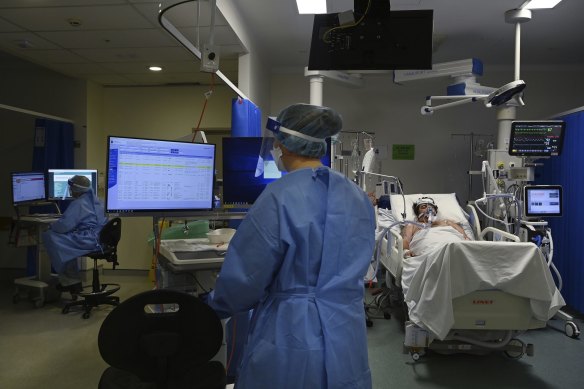
ICU wards such as St Vincent’s hospital in Sydney are seeing more young patients presenting with severe illness during this wave.Credit: Kate Geraghty
When someone is sick with COVID or isolating, they are often placed into hotel quarantine now, too, to reduce the risk to their household. During this Delta outbreak, NSW officials have said the secondary attack rate (how many other people get sick once there’s a case in a home) has climbed from 25 per cent earlier in the pandemic to almost 100 per cent. “Alpha was still containable with our usual measures,” says Benett. “We just had to work harder, this one needs more than that.”
A federal government spokeswoman says that the definition of close contacts has been refined throughout the pandemic and, as no single infection control measure is a guarantee, many work together, under routine review by the government’s expert advisory committee, the AHPPC. In Queensland, where recent leaks from hotels have put the state into snap lockdowns too, Dr Young says this: “We know the Delta variant presents significant challenges to hotel quarantine”, but she says the state is using CCTV surveillance to minimise security on guest floors, and N95 masks and eye protection for staff. Victorian and NSW health authorities did not respond to requests for comment before deadline.
Duckett says best practice needs to keep evolving but he’s not sure a national set of rules for containing the Delta variant, as called for by some experts in recent days, is the answer. “It’s the states you want running things and they’re already talking to each other,” he says. When asked in July about a national approach to Delta, federal Health Minister Greg Hunt said the AHPPC was meeting nearly every day to discuss common approaches and national standards, which could then be applied to specific outbreaks. “The [more-infectious] Delta variant ... has created some of the next evolution of responses through the national cabinet and as a result of that right now everybody’s pitching in,” he said.
But is the outbreak all because of Delta? And can we defeat it?
The NSW government has drawn criticism for not locking down earlier once the Delta variant was first identified and for allowing a looser shutdown than those interstate, with some retail still open. “The amount of Bunnings that are exposure sites,” says Toole. “The Premier just keeps saying it’s Delta. But it’s complacency to blame too. And that’s the story right across Asia. These places which were once the envy of the world like South Korea, Vietnam [for early containment] are now having outbreaks and they’ve been too slow to vaccinate.”
Duckett adds that outbreaks hinge on both luck and management. Some people don’t spread the virus as well as usual; others can be “super-spreaders” and infect many more than expected. “In NSW this time, they’ve had both bad luck and they’ve been too slow to lock down,” Duckett says. When they said they were surprised by the fleeting contact [spread], they shouldn’t have been. They knew it was Delta ... We had tough lockdown rules in Victoria and the graphs show what happened. It worked.”
Australia has beaten Delta before, at least on a small scale, such as in Victoria and Queensland in June. (Both states are now dealing with fresh breakthroughs by the virus.) When scores of fly-in-fly-out miners boarded planes last month around the country after being exposed to a Delta case at a Northern Territory mine, much of Australia found themselves under snap lockdowns but that cluster has not spiraled out of control as feared. Still, Victoria’s Chief Health Officer Brett Sutton notes his state was in lockdown when it beat back Delta last month, due to another “absolute beast”, the Kappa variant, and has said there is no guarantee “we can win against Delta” and drive cases back down to zero. Experts say NSW, in particular, remains in trouble.
Modelling by the Burnet Institute, factoring in Delta’s higher reproduction number, has found NSW could bring down cases if it moved to a Victorian-style harder lockdown. But Premier Gladys Berejiklian says that, although the numbers are still “bouncing around”, they do not seem to be growing exponentially.
“We’ve never really quashed an outbreak like this so it needs to be hard...and we can’t just let it rip either,” Toole says.”India is finally starting to get Delta back down but it’s now getting out of control in places like the US and the UK.”
While experts say Australia has done well at stamping out the virus so far during the pandemic (and may yet triumph over this Delta outbreak too), our vaccination rates lag behind the rest of the developed world and that leaves us vulnerable to emerging variants. “It’s not the variants of concern really, it’s the lack of vaccination that’s the concern,” says Vasan.
“If we hadn’t messed this up, we probably wouldn’t be at herd immunity yet, but we’d be in a much happier place,” Duckett says. ”There’s going to be other variants, we’ve got to be ready.“
What do emerging variants mean for the pandemic?
As viruses better adapt to a species, they generally become less deadly but more infectious over time. “A virus that always kills its host will end up with nowhere to go,” Toole says. “Viruses don’t have brains but they’re strong survivalists.” Sometimes a virus will beef up its potency to jump a barrier, which could lead to more severe disease. But Vasan says they generally stabilise over time.
“These variants we see now are neither over-hyped nor cause for panic,” he says. With the virus forced more and more into corners by lockdowns and vaccinations worldwide, running out of new hosts to infect, it was always expected to evolve. “It’s only a matter of time before we have more variants of concern, I wouldn’t be surprised if there was another before the end of the year. There’s a few variants we have an eye on, variants of interest we call them, like Lambda. But the virus is still not mutating as fast as, say, flu. We need a new vaccine against that every year.“
Still, rich nations hoarding vaccines supplies mean it’s likely much of the developing world will be unvaccinated for some time – and more likely variants will mutate in those populations. Toole says Delta is a warning shot, a sign we have crossed into a dangerous new phase of the pandemic where the virus is evolving faster but vaccination coverage is still not at the majority needed to slow its spread.
Experts expect more outbreaks will continue until it is. “I almost think Delta marks the end of COVID zero [elimination],” Bennett says. “Even if we do contain this outbreak, the chances of doing it over and over again with that variant are very low. And one may get just another slight edge that means we can’t contain it at all. We’ve been too relaxed in Australia, but now the virus is dictating the timing again and we can’t just open our doors either and let it back in until [vaccination] increases.”
Toole and Duckett agree vaccination and hotel quarantine must be improved, as our first line of defence. “It’s our moat but at the moment it’s empty of water,” says Toole. “You can jump right across it. And Delta has.”
Let us explain
If you'd like some expert background on an issue or a news event, drop us a line at explainers@smh.com.au or explainers@theage.com.au. Read more explainers here.