Explainer
- Explainer
- Coronavirus pandemic
Speckled monsters and graverobbers: what can we learn from the killer plagues of history?
What happened during past pandemics? Why do outbreaks keep happening? And how might COVID-19 end?
They must have felt like nightmares, those plagues of the past. When sickness came, it seemed to come from nowhere, carving off huge swathes of the population as if at random. Was it divine intervention, an internal imbalance, ill-humoured vapours rising from the Earth?
By the late 19th century, scientists had found and named the culprit. Invisible though they are to the naked eye, microbes have killed more people throughout history than war. They are the tiny invaders (germs such as viruses and bacteria) that unleash disease. They’ve led us to riot and murder but also to art and innovation. Much of modern medicine, from vaccinations to germ theory itself, took root in the panic of a pandemic. In cities such as Venice, where the quarantine measures we now know so well were born under the medieval waves of the Black Death, plague paintings still soar overhead in churches built by its survivors.
Some outbreaks, such as influenza, malaria and HIV, now linger in our lives; others, notably smallpox, have been beaten into extinction or somewhere near it. This time, the disease on the loose is less deadly than the first dangerous coronavirus to emerge in the modern era, SARS, but it’s also more infectious. While SARS made it into less than 30 countries before it was stamped out (over nine anxious months) in 2003, it took COVID-19 less than 12 weeks to morph into the first major pandemic to hit the world since Spanish flu a century ago.
So what can we learn from the outbreaks of the past? What clues do they leave us about how COVID-19 will end? And is humanity really getting better at handling infectious disease?

During the plague of London in 1665, a doctor in 17th-century personal protective equipment slides bodies into a grave. The rat-borne bacteria that cause bubonic plague are in colour. Credit: Getty Images. Composite: Mark Stehle
When did pandemics start happening?
Disease has always stalked humanity but pandemics – the significant worldwide spread of a pathogen – are a modern phenomenon, says Professor Frank Ruhli, who heads the Institute for Evolutionary Medicine at the University of Zurich in Switzerland. He’d know – a lot of his work days are spent poring over ancient mummies to crack the cold cases of diseases past. The molecular proof of a germ tends to break down fast in fossils, Ruhli says, but, even in prehistory, there were outbreaks. The difference was that because we lived spread out in small groups of hunter-gatherers, the new pathogen of the day tended to fade just as quickly as it emerged, having run out of people to infect.
Then, as the world opened up to large-scale trade and travel roughly 6000 years ago, Ruhli says, viruses suddenly had an easier way to cross borders, countries, even continents. “Now, today, a virus can get on a plane and go global within 24 hours."
Sir Richard Evans, provost of Gresham College in London, is a leading authority on the great plagues of our past. He says you don’t need a magic number of people before a pandemic can take hold; rather, you need a way for a disease to reach unfamiliar populations, perhaps marched in by an invading army, hitching a ride on a railway or docking with a ship from another land. "In 1492, Christopher Columbus took smallpox to the Americas and returned to Europe with syphilis," Evans says. (Columbus, it turned out, came off better – the pox had long ravaged European populations but left survivors immune, giving them an advantage over the Indigenous peoples of the Americas and even Australia, where "the speckled monster" wrought a devastating toll.)
Even today, well-established diseases can "break out" again when long-isolated communities in remote corners of the world at last collide with modern civilisation. During the 1950s and '60s, a group of Yanomami people living in Brazil were nearly decimated by measles after making contact with the outside world; a Yanomami teenager has now tested positive for COVID-19 as fears grow for Indigenous people across the world.
The Black Death wiped out more than a third of Europe's population over just four years.
As we are seeing in the case of COVID-19, much about how a pandemic unfolds is up to the germ. Does it jump from person to person, travel through the air or thrive in contaminated food or water? But the lifestyles and responses of those afflicted – even the accidental kind – play a role too.
One of the world's earliest plagues, likely of typhoid, bred in the cramped, squalid conditions of a city under siege as Sparta attacked Athens around 430BC. Seeing the smoke from funeral pyres rising over the walls, those invading troops very smartly went home (possibly to self-isolate). While the contagion did return again, and again, it did not spread far beyond Greece.
Then, in the fifth century, the Roman Emperor Justinian’s conquest of Mediterranean brought a tiny bacteria all the way out of Egypt and into the heart of Europe, igniting what is often considered the world’s earliest pandemic, the first wave of the bubonic plague. Its toll was so devastating some even credit it with bringing down the Roman empire. Having wound its way out of Asia along the Silk Road, it would return for at least two more pandemic hits, including the Black Death that wiped out more than a third of Europe's population over just four years in the 14th century.
Overall, the bubonic plague remains history’s biggest killer – between 75 million and 200 million people were felled by it before the 20th century, and even today it rears its head from time to time. But we know its secret now: the disease is spread by bacteria that live on the backs of rats, and we have both antibiotics and a vaccine (of limited availability) to treat it.
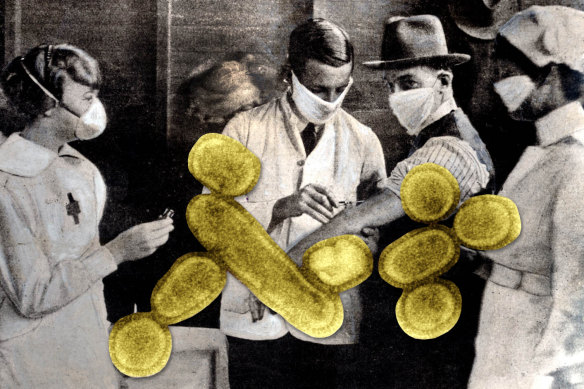
At the Hyde Park Inoculation Depot in Sydney a man is vaccinated against H1N1 virus that caused Spanish flu.Credit: Getty Images. Composite: Mark Stehle
How have societies reacted to past pandemics?
Down the pandemic records, much of humanity's responses have been guided by instinct if not science, Ruhli says, a memory gene deep. Just as our body tells us to run when we see a tiger stalking through the jungle, we also know to keep away from the sick as much as we can. In some parts of medieval Europe, whole cities were built around the idea of isolation.
"It was recognised by the Renaissance period that diseases did travel," Evans says. To stop it, ships arriving in Venice during a wave of plague in the 15th century were forced to sit at anchor under the first quarantines – a period of 40 days or quaranta giorni in Italian, hence the word quarantine.
"It's why you see people [panic] buying toilet paper now, there's a selfish evolutionary imperative to protect yourself," Ruhli says. "But humans also live together in groups so there's altruism built in too. In this pandemic, we are seeing the whole range of behaviour from the idiot who steals masks and hand sanitiser to the healthcare worker risking their life to care for the sick."
Even the pharaohs of ancient Egypt were not immune. The same infectious bugs that struck down commoners took out their kings too.
Often pandemics were blamed on outsiders or on poverty and the "great unwashed" poor. Bad hygiene, a common concern in slums where people are packed in close together without access to proper sanitation, does play a role in most infectious disease transmission. Contaminated food and water carried the great cholera outbreaks throughout history, Evans notes. But disease does not discriminate by class or race. Even the pharaohs of ancient Egypt, revered as gods, were not immune. Ruhli has found the same infectious bugs that struck down commoners took out their kings too.
Evans notes authorities have never coped particularly well with pandemics, even when authoritarian states already had extensive powers to control people's movement. "There's always been a tension in government between fear of economic disaster and fear of epidemics," he says. "In almost every pandemic, authorities initially refused to report the outbreak, in case it led to panic on the exchange, or the crippling of trade." In Hamburg in 1892, he says, the refusal of the Senate to report deaths on the waterfront from cholera saw 10,000 people die in just six weeks.
In the early days of COVID-19, China tried to cover up and downplay the outbreak – as it did, to a much greater extent, during the SARS epidemic 20 years earlier. Then, this time, as the new coronavirus exploded, China did something without precedent in our modern era – it locked down more than 10 million people in an effort to starve the virus of new hosts. That move, while fairly successful so far, has proven challenging to replicate in democratic societies. Italy hesitated long enough to give the virus a foothold; by March, its hospitals were overrun.
Still, even when governments have tried to follow the medical dogma – with case isolation and social restrictions – it hasn't always been well received. Russia sealed off its slums when cholera hit during its second great pandemic of 1829. That slowed the spread but the sick (and sometimes even those who weren't) were largely left to fend for themselves. In 1831, as rumours swirled that the lockdowns were a Tsarist plot to kill off the poor, violent riots broke out, with doctors the main targets.
Evans notes that, in Hamburg, where respected medical scientist Robert Koch helped deliver the message on the need for containment, the streets were quiet. Meanwhile, there were also riots in London as authorities struggled to contain the disease. Graverobbing scandals involving scientists – and revelations of two serial killers selling bodies to a local anatomy school – fuelled stories that cholera victims were being taken away to be murdered for experiments. In the end, an appeal from another respected doctor calmed people. Riots have also broken out alongside more recent outbreaks - such as in 2010 when UN peacekeeping troops brought cholera to Haiti.
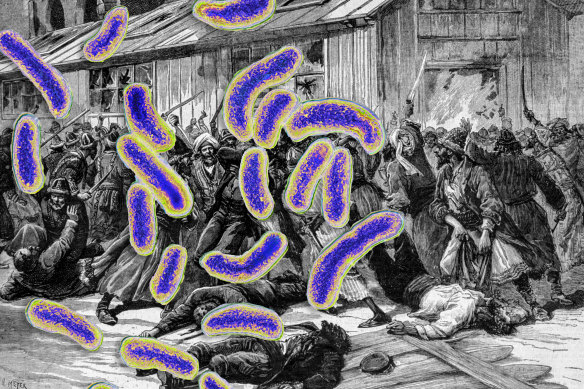
The cholera bacteria superimposed on riots over quarantine measures in Astrakhan, Russia in 1892.Credit: Getty Images. Composite: Mark Stehle
How did past pandemics end?
Most diseases, once loose, tend to linger in some form in humans. But there are two main ways a pandemic wave comes to an end, says Nobel Prize-winning immunologist Professor Peter Doherty. The old road of early history saw infections burn out once enough people had either died or recovered with natural immunity then encoded into their cells. The other way is intervention – quarantine and, today, medicine.
Back in the Middle Ages, when the plague kept returning, there wasn't a choice. Without a treatment or an inoculation, survivors could only avoid the sick via quarantines and hope (and pray) they would be spared next time the Black Death came to call. Their DNA helped shaped the evolution of the human immune system. But scientists stress that we still don't know how long or even if survivors of COVID-19 will likewise become immune. This is a "virgin soil" pandemic, Doherty notes, brand new to humanity. So "letting the virus rip" in order to build up a faster "herd immunity" against it, could be catastrophic, especially given its mortality rate seems at least 10 times that of seasonal flu.
In the case of the other main killer in history, smallpox, the turning point came in 1796. The virus is from the same family as the less severe cowpox and monkeypox and is thought to have first emerged around the time humans began domesticating animals (it was found in the tombs of ancient pharaohs, Ruhli says). Last century, it became the first human disease to be wiped off the face of the Earth. How? English doctor Edward Jenner had observed that milkmaids with cowpox tended not to be stricken by smallpox. He took fluid from a cowpox lesion and injected it into the arm of a nine-year-old boy before exposing him to various viruses. The boy didn't ever catch smallpox and so the modern method of engineering immunity against disease began. But it would take almost another 200 years to drive out the pox altogether as some countries held out against mandatory inoculations.

Edward Jenner who discovered vaccination against smallpox (seen here in colour).Credit: Getty Images: Composite Mark Stehle
The 1918 Spanish flu – to which this new pandemic is now being routinely compared – killed more people than World War I, which was just drawing to a close when it emerged. Both Doherty and Professor Marc Pellegrini, an infectious diseases clinician at the Walter and Eliza Hall Institute, say parallels to that H1N1 influenza strain are fair but both hope this new pandemic will prove less deadly now medicine has advanced. "Still, global travel has really changed how pandemics operate, this isnt going away yet," Pellegrini says.
The Spanish flu didn't burn out for at least two years (having come not from Spain but likely China, France or even the US). Perplexingly, the people struck down were often in their prime rather than the very young or old typically hit by influenza. And, as the disease arrived before the age of antibiotics, secondary bacterial infections likely killed more people than the virus itself. Evans notes it was also malnourishment and poor hygiene in overcrowded medical camps that pushed the death toll to 50 million worldwide.
Some priests weren't allowed to give the last rites and, in Tasmania, pubs could let in only three people at a time for five minutes each.
As with COVID-19, the mutant flu strain was very infectious, jumping from person to person in close quarters, and so society largely shut down to contain it. "It was really the birthplace of [modern] public health," Ruhli says. The US city of Philadelphia took a now-notorious 14 days to react after its first case, even pressing ahead with a big public march to celebrate the war effort. St Louis, meanwhile, cracked down on people's movement and gatherings within just two days of the influenza strain entering its borders. By the end of the crisis, its death toll was less than half of Philadelphia's, even though a second wave of infections hit it a little harder.
Australia held out longer than most of the world under strict land and marine quarantines. But by 1919 the virus had found a way in, including in the lungs of soldiers returning from war, and went on to infect millions. People were often outraged by the new social restrictions – some priests weren't allowed give the last rites in quarantine zones, forgetting your mask was a fineable offence and, in Tasmania, pubs could let in only three people at a time for five minutes each.
Are we getting better at handling pandemics?
Before COVID-19 – three years ago, in fact – US infectious diseases expert Michael Osterholm said there had never been a more daunting time to control an outbreak than the modern era. Why?
While medicine might be more up to the task, the likelihood of a spillover – in which a new virus jumps species lines into the human race – is more likely than ever. Humans are in more places than ever before and, as we churn through the last pockets of the wild, clearing forests and poaching wildlife, we collide with more species.
Nowhere is this more obvious than in the case of wet markets still popular throughout Asia. Such markets are notorious breeding grounds for disease as stressed animals from all corners of the world are caged close together, trading unfamiliar diseases, and then handled and butchered by humans.
SARS was traced back to a colony of bats but was believed to have passed into humans in a wet market via the Himalayan palm civet, an ancient species of mammal often eaten as a delicacy. And MERS also has bat origins but mostly spreads from infected camels, including in slaughterhouses. A wet market is again the prime suspect in the COVID-19 outbreak, leading authorities including the United Nations and the Australian government to call for their permanent global shutdown.
In the face of repeated warnings from scientists that a pandemic was coming, the world did very little to prevent it.
Ruhli muses that because of our ancestry as hunter-gatherers, living from one day to the next, much of our brain is wired to deal with immediate dangers. We're not the type of species to stockpile for a rainy day. "At least not ordinarily", he laughs. This helps explain why the world has responded so quickly to this crisis, he says, with the extraordinary lockdown measures experts called for but has struggled to avert the likely more serious but less immediate threat of climate change.
Likewise, others have pointed out that in the face of repeated warnings from scientists that another pandemic was coming – as more SARS-like viruses were discovered in the wild and the illegal wildlife trade boomed – the world did very little to prevent it.
“In certain ways, [as a species] we’re still in the Stone Age. We can’t deal with the spread of [disease] like this," Ruhli says.
Doherty says the world was starting to head in the right direction when COVID-19 arrived, having launched a rapid pandemic response vaccine program, CEPI (the Coalition for Epidemic Preparedness Innovations), in 2017, with coronaviruses even earmarked as a priority. But in hindsight, he says there should have been a similar accelerator set up for reactive drug therapies too, and the hunt for a cure to SARS should not have stopped just because the virus vanished.
Such drug therapies have helped bring the other pandemic of the modern era, HIV/AIDS, into line, even if it is still with us. Against a virus without a clear cure, which writes itself permanently into a patient's DNA, vaccines have so far failed. But scientists have developed ever more efficient drugs to stop HIV killing once inside the body.
As Ruhli puts it: “We are in a constant arms race against pathogens.”
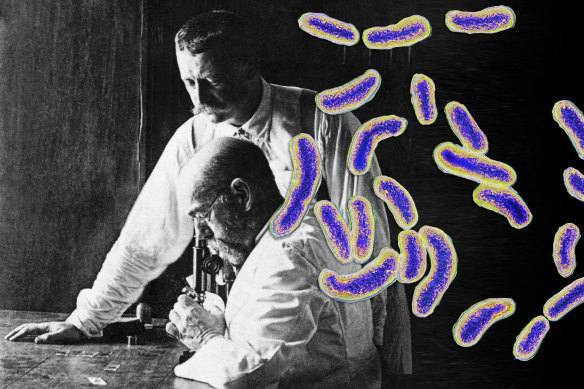
Robert Koch, seated, the founder of bacteriology and discoverer of the cholera (pictured) and tubercular bacillus with his oldest student and assistant, Richard Pfeiffer.Credit: Getty Images. Composite: Mark Stehle
So how might the COVID-19 pandemic end?
Almost all experts are hesitant to guess. While there are lessons and patterns down the years, mutating virus strains are notoriously full of contradictions. "This pandemic is writing its own history," says Pellegrini.
The virus shares about 75 per cent of its DNA with the strain behind the SARS outbreak, so it's often called SARS 2. Yet Pellegrini says it's not behaving quite like that virus either - less deadly but more infectious and spreading further by stealth or asympomatic cases (as was observed to an even greater degree during long-running outbreaks such as polio). "It aint going away any time soon," Pellgrini sighs. "Even if we get rid of it soon, I have no doubt in my mind there will be a SARS 3. But we're throwing anything we have at it."
A lot of the world's preparation for COVID-19 is based on a more familiar foe: influenza. As another contagious respiratory illness, the new virus is similar in some ways to the flu but different (and more dangerous) in others - and scientists are now racing to determine just how much it might diverge from the modelling. This will help them answer key questions: whether it is possible to eliminate the virus entirely through lockdowns and aggressive case detection, as New Zealand is aiming to do; or whether it's already time to open up again for business.
During the 1918 flu pandemic, when Australia and most countries relaxed similar social restrictions, the virus hit again in a second wave. This time around, Singapore became an early success story, "flattening the curve" of rising caseloads but, when it eased restrictions, the numbers shot back up and have kept climbing. Even China might be seeing the start of a second wave outbreak after lifting lockdowns.
Coronaviruses are much more stable than the wildly unpredictable genetic code of influenza.
With a vaccine for this bug still likely 12-18 months away, experts are encouraged by the prospect of developing an effective treatment or even preventative drug along the lines of a HIV therapy that could stop an infection taking hold in the first place. During the swine flu pandemic in 2009, experts say two anti-virals that already worked on the illness helped keep the death toll relatively low, even though it spread to about 20 per cent of the world's population. Several contenders have already been pulled from the existing medicine cabinet and are now being trialed in COVID-19 patients around the world, including in Australia.
Of course, there is the more terrifying prospect that a vaccine doesn’t work or the pathogen mutates to evade our immunity, evolving and lingering like seasonal flu, Doherty admits. Most researchers, Doherty among them, think it very unlikely the virus will morph into something nastier – by its very nature, a virus wants to spread rather than kill and coronaviruses are much more stable than the wildly unpredictable genetic code of influenza.
Usually, a virus will beef up its potency to jump across species lines – say, from animal to human. Over time circulating in a new population they tend to lose more of their bite – as has already happened with Swine flu, the 1918 flu and the four most common coronaviruses. Today those four only give humans mild colds and coughs.
But, as Doherty suggests, "When they first jumped [from animals] into people they probably hit us just as hard as this."
Sign up for our Coronavirus Update newsletter
Get our Coronavirus Update newsletter for the day’s crucial developments at a glance, the numbers you need to know and what our readers are saying. Sign up to The Sydney Morning Herald’s newsletter here and The Age’s here.
Let us explain
If you'd like some expert background on an issue or a news event, drop us a line at explainers@smh.com.au or explainers@theage.com.au. Read more explainers here.