- Exclusive
- National
- Coronavirus pandemic
This was published 5 years ago
The perfect virus: two gene tweaks that turned COVID-19 into a killer
By Liam Mannix
If you were to hold a horseshoe bat in your hand, it would barely fill your palm, and weigh little more than a ballpoint pen.
The creatures live in the darkness. Their name comes from their oddly-shaped noses, which look like upward-pointed horseshoes. Generally we ignore them and they ignore us.
In 2013, in the Chinese province of Yunnan, about 2000 kilometres south-west of Wuhan, a horseshoe bat was caught in a trap. Chinese scientists swabbed its mouth and checked the saliva for virus genes.
Bats’ tiny bodies teem with viruses. But this bat had a virus researchers had never seen before. It was a coronavirus, and it looked a lot like SARS, a virus that had spread around the world rapidly a decade earlier and then vanished without a trace.
But this virus infected only bats, not humans. The researchers named it RaTG13 and then promptly forgot about it.
At the same time, other research groups noted these bat coronaviruses regularly seemed to jump from animals to humans, and posed a significant pandemic threat.

In 2013, in the province of Yunnan, about 2000 kilometres west of Wuhan, a horseshoe bat was caught in a trap.
And then ... the world moved on. We had bigger things to worry about than Chinese bat coronaviruses.
It is now clear we made a mistake.
The virus that is causing the first pandemic in 100 years – it will likely kill millions before this is all over, and mean that life may never be the same again – shares 96 per cent of its genetic code with RaTG13.
“We have been monitoring these coronaviruses. They’ve been jumping species boundaries,” says Professor Edward Holmes. “We knew this was going to happen.”
RaTG13, or another very similar bat virus, has managed to pick up two tiny genetic tweaks that turned it from a bat disease into a virus perfectly adapted to make humans sick.
Then it had the unbelievable misfortune to emerge in exactly the wrong place at exactly the wrong time.
“It’s got this beautifully adapted set of mutations,” says Holmes. In his published work, he calls it a “perfect epidemiological storm”.
A crown of spikes
Holmes, a researcher based at the University of Sydney, is among the world’s leading experts on the genetics and evolution of SARS-CoV-2, the virus that causes COVID-19.
He was on the team that first sequenced the genes of the virus from one of the first patients in Wuhan. Their article on the possible origins of the virus is now the most-publicised Nature study in the history of that venerable journal.
He has visited the Huanan seafood and wildlife market where the Wuhan outbreak began. He has visited caves in China, searching for bats so he can survey the viruses they contain.
CoV-2 is a coronavirus, just like SARS and MERS. These viruses get their name from how they look under a microscope: a tiny bubble of fat surrounded by a crown of spikes which are used to penetrate cells.
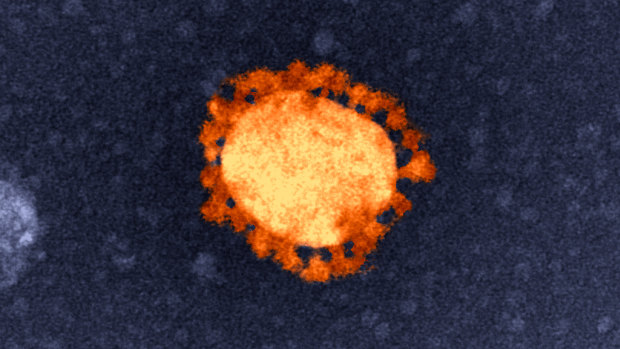
An electron-microscope image of the COVID-19 virus, isolated from the first Australian coronavirus case. Note the bubble in the centre surrounded by spikes.Credit: CSIRO
Animals have many different types of viruses. But coronaviruses seem uniquely able to jump from animal to human. “They just have this ability,” says Holmes. We don’t know why.
The emergence of SARS in 2003, killing 774 people, should have been a warning: these viruses jumped, and when they did lots of humans died.

CSIRO comparative immunologist Michelle Baker. Credit: CSIRO
We should have started building broad-based vaccines and antivirals that target all coronaviruses.
Instead, SARS was defeated largely by enhanced hygiene measures. Several drugs and vaccine candidates for SARS were developed and then largely abandoned.
“We have been completely complacent,” says Dr Michelle Baker, the CSIRO’s leading bat virus researcher.
“It gets really difficult to get funding when there is not an outbreak. People feel a sense of security. They don’t feel it’s relevant anymore.”
Why this virus?
The virus pulled from bats in 2013 could not infect humans. SARS-CoV-2 can. Why?
It appears that two tiny tweaks to the virus’ genetic code have made a huge difference.
CoV-2 wants to do two things: bind to a human cell and then get inside it. The virus binds to a cellular receptor – think of them as little antennae that stick off the side of human cells – called ACE2.
ACE2 receptors are designed to listen for signals that change our blood pressure. Fine adjustments to blood pressure are really important in our lungs, so our lung cells are covered in ACE2 receptors.
SARS was able to bind to ACE2. But small genetic changes mean CoV-2 binds almost perfectly, at least 10 times more tightly than SARS. “It’s beautifully adapted to do that,” says Holmes.
But that’s not enough. Once CoV-2 is stuck on a cell, it needs to get in. That’s where the second tweak comes in.
CoV-2 is covered in spikes. They act like tiny harpoons. The virus needs to stick to the cell and then fire a harpoon. The harpoon pulls the surface of the cell and the virus together, allowing them to fuse. That’s how the virus gets inside.
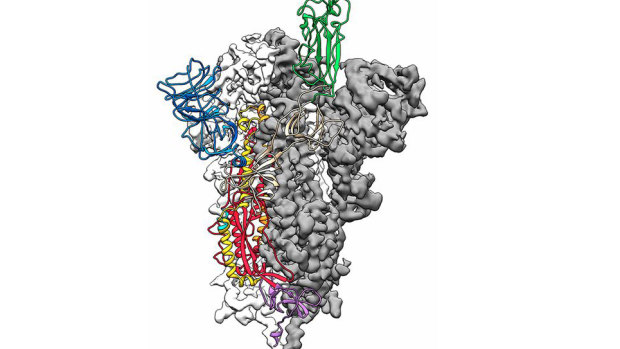
A 3D map of the virus's spike protein, which it uses to 'harpoon' human cells. Credit: Science
“But you don’t want the harpoon firing off randomly,” says Professor Stephen Turner, head of microbiology at Monash University. “You only want it to fire when it’s ready to infect the cell. If it’s going off too early or too late, the virus would not be able to infect us.”
To trigger the harpoon at just the right time, viruses rely on human enzymes, little proteins in our blood. Some enzymes trigger the harpoon too early, others trigger it too late. Among the best enzyme triggers – the one that fires the harpoon at exactly the right time – is an enzyme called furin. Our bodies produce heaps of furin.
“Basically, you can work out if a virus is going to be highly pathogenic or not if it is activated by furin,” says Turner.
Bird flu is triggered by furin. We got lucky, though, because it wasn’t very good at sticking to our cells. CoV-2 is great at sticking to our cells. And it’s triggered by furin, among the best triggers a virus can have.
“The combination is what makes it so infectious,” says Turner.
The birth of a virus
How does a bat virus pick up these tricks?
Bats live essentially symbiotic relationships with their viruses. The viruses don’t want to kill the bats, because then they’d have nowhere to live.
When scientists test bats, they find lots of different viruses but at very low levels. “Often it’s really difficult to find a virus in a bat,” says Baker.
And these viruses are, in evolutionary terms, very stable. They don’t change much. It is unlikely RaTG13 turned into SARS-CoV-2 within a bat, Baker says.
But things change when a bat virus jumps to another animal.
Here’s one potential scenario.
RaTG13 has the ability to bind to ACE2. But it did not have the furin tweak which makes the virus so infectious.
It is possible RaTG13, or a similar virus, jumped from a bat into a pangolin – a small, scaly anteater common to Asia and highly valued in traditional Chinese medicine.
Pangolins also have the ACE2 receptor, as do other animals like ferrets.
Either of these animals, or many others, could have been the middle animal between bats and humans.But in this particular origin story, the pangolin was infected at the same time with another bat coronavirus. This virus possessed the furin tweak.
When two viruses infect the same host, they can ‘recombine’ – swapping their genes.
This may have created a virus that could both stick to ACE2 and use furin to quickly get inside human cells. That could have been how SARS-CoV-2 was born. Then it jumped to humans in the close confines of the Wuhan wet market.

An image of a bamboo rat caged on top of a deer allegedly sold at the Wuhan seafood market has circulated online. Credit: Weibo
And Wuhan is the perfect spot for a virus to jump. The city is home to millions. It is an international travel hub. The virus appeared just before the biggest travel period of the year: the Chinese Spring festival.
That story is neat. But it is no certainty. The first documented COVID-19 patient had no exposure to the wet market.
It is possible, although unlikely, this virus was circulating in humans for years before breaking out into a pandemic.
It could have spread silently, causing only mild cold-like symptoms, before suddenly acquiring a key mutation or two that made it much more contagious - and much more dangerous. “You cannot rule that out,” says Holmes.
“Whether that market was involved or not, it’s really unclear at the moment. We may never answer that question.”
‘We need to change the way we live’
Holmes is shocked at how fast SARS-CoV-2 has spread. But he’s not shocked it was a bat coronavirus that caused a worldwide pandemic.
Environmental damage, illegal wildlife trading (pangolins in particular are heavily traded), wet markets and the climate crisis are all combining to push humans and bats closer than ever before.
“It is blindingly obvious that we as humans have to change the way we interact with the animal world. There is no doubt about that,” he says. “And it’s not the animals' fault.
“Bats have been carrying these viruses for millennia. It’s not them that’s changed, it’s us – the way we interact with them.
“The whole world is now set up for a pandemic - we live in megacities, there is transport. It’s an accident waiting to happen, and it happened.”
When the world eventually starts to recover from the pandemic, steps need to be put in place to widen the gap between bats and humans so this cannot happen again, Holmes says.
“We have to cut our exposure. Those markets have to go,” he says. “The illegal trade in wildlife has to end. We have to cut our exposure. That’s very very clear.”