This was published 2 years ago
Charlie Teo, the profit of hope: How neurosurgeon left families with a terrible price to pay
A year-long investigation reveals the devastating impact on families of ultimately futile procedures conducted by the renowned brain surgeon.
By Kate McClymont and Thea Dikeos

Neurosurgeon Charlie Teo.Credit: Charlie Teo by Gary Heery / X Portraits
Controversial neurosurgeon Charlie Teo has charged families extraordinary amounts of money for ultimately futile operations that have catastrophically injured patients, a joint Sydney Morning Herald, The Age and 60 Minutes investigation can reveal.
Several families, including those with young children who were left in a vegetative state, have spoken out about the dreadful price they paid for the hope Dr Teo sold them.
“There should be some regulation to stop this. If someone is giving false hope, then it’s like a scam,” said Prasanta Barman, who is plagued by guilt, following the horrific outcome of the futile surgery Teo performed on his only child.
In mid-September 2018, Barman, an engineer from Assam in India, was worried when his son, four-year-old Mikolaj, appeared to have difficulty walking.

Mikolaj Barman (centre) was diagnosed with a very rare type of tumour – a diffuse intrinsic pontine glioma (DIPG). He is pictured with his father, Prasanta, and his mother, Sangeeta.Credit:
He and his wife Sangeeta were devastated when their son was diagnosed with an incurable and inoperable diffuse intrinsic pontine glioma (DIPG). A second neurosurgeon confirmed the diagnosis.
Desperate for a miracle, a friend emailed the famed Australian neurosurgeon on his behalf, saying: “The doctors in Delhi have told him [Barman] that no treatment is possible” and they were hoping that “a Western doctor can offer his son a lifeline”.
Teo, 64, is arguably Australia’s best-known neurosurgeon. He is renowned for his aggressive surgical style, especially in cases other surgeons deem inoperable, and he has many grateful patients who laud his successes.
In the media, he is often portrayed as a maverick, motorbike-riding outsider fighting against both the medical establishment and his colleagues who, he suggests, are jealous of his superior skills.
In 2021, Teo had restrictions placed on his ability to perform brain stem operations and faces a disciplinary hearing over two poor surgical outcomes, one of which was a DIPG.
On September 27, 2018, Barman was elated when what seemed like a lifeline was offered. “Dr Teo has reviewed the scans and suggested urgent surgery, he said there is a very high likelihood of cure if he does the surgery before radiation,” the email from Teo’s office in Sydney said.
The following day, replying to Barman’s questions about the prognosis and risks, Teo’s office emailed, saying: “If all goes as planned, the surgery should be curative as we should be able to remove the entire thing. This means that prognosis would be excellent … He should hopefully live a long and happy life.”
However, there is no chance of a happy ending with a DIPG, the most lethal of all childhood cancers. There is no cure and the average life expectancy from the time of diagnosis is between six and 18 months.
“It is the only tumour in paediatrics where, from the day you’re diagnosed, you’re already considered palliative,” leading American paediatric oncologist Mark Kieran told the joint investigation.
“It’s not just a question of if you are going to die, it’s really when you’re going to die.”
Kieran said any attempt at resection or removal of a DIPG could only result in “neurologic devastation and eventual death either from the surgery or your tumour”.
Asked if there was any clinical or research data anywhere in the world that shows a benefit from resecting DIPGs, one of America’s pre-eminent paediatric neurosurgeons, Professor Mark Souweidane, said bluntly: “Absolutely not, doesn’t exist.”
Souweidane, head of paediatric neurosurgery at the Weill Cornell Medicine Brain and Spine Centre in New York, has been researching DIPGs for more than two decades. He said surgery is not and has never been an option for this uniformly fatal brain tumour and that it would be “incomprehensible” for anyone to attempt this.
There should be some regulation to stop this. If someone is giving false hope, then it’s like a scam.
Prasanta Barman
The professor explained that because the aggressive tumour has infiltrated the pons, “the part of the brain that decides when you breathe and when your heart beats”, any attempt at resection will result in devastating consequences for the child.
“To go in and remove that area would remove the very part of the brain that keeps you alive.”
Barman explained to Teo that he had no medical insurance, so he would have to meet all the costs himself.
He was informed that the operation would cost $150,000 at Prince of Wales Private Hospital in Sydney or $80,000 in Singapore, of which $40,000 would have to be in Teo’s bank account before surgery.
Barman sent another email to Teo asking the famous neurosurgeon to double-check the two MRIs to “make sure about the certainty of the operation” because the opinion of the two Indian neurosurgeons was that “there is no treatment for this type of tumour. This is very rare. And once detected, we’ve got only eight to 12 months in our hand,” Barman recalled.
But Teo begged to differ. “Our diagnosis and recommendation remains the same and we think we can cure Mikolaj with surgery,” said the emailed response from Teo’s office to Barman.
When he read Australian press reports describing Teo as “a miracle worker”, Barman was reassured that the much-hyped doctor could deliver the cure he was offering.
That same day, Barman’s friend set up a GoFundMe page to help with the steep costs for the operation to remove Mikolaj’s DIPG in Singapore.
The crowdfunding page referred to the tumour as “inoperable”.
“However there is hope. A renowned Australian neurosurgeon, Dr Charlie Teo, believes he can successfully remove the tumour using a pioneering technique. With this treatment, Mikolaj’s prognosis would be excellent, and he will hopefully live a long, normal life,” read the crowdfunding page.
Barman drained his savings and his retirement fund, Mikolaj’s school helped and friends donated money for the operation on October 11, 2018. Photos taken the night before the operation showed the happy, lively boy in his hospital bed surrounded by colourful balloons, playing with his toys.
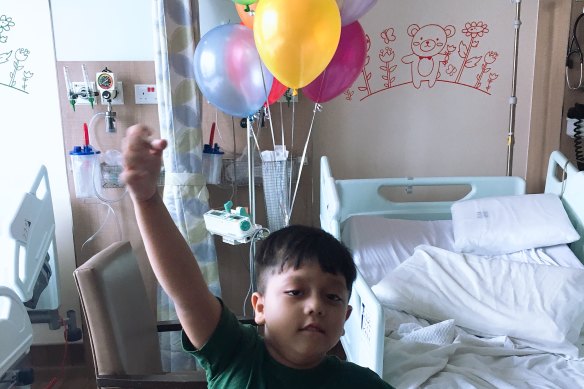
Mikolaj Barman playing with balloons the day before his operation.Credit:
His father told him, “There will be a big fight tomorrow, there’s something inside your brain, something inside your head, so that bad things will be taken out, and after that you’ll be OK again.”
Barman wiped away tears as he recalled what were to be among his son’s last words. Mikolaj told his parents he was ready for battle and, punching the balloons, the little boy said, “I will fight like this”.
Teo only met the young child for the first time as he was being wheeled into the operating theatre at Singapore’s National University Hospital and only half an hour before the operation, he broke the news to Mikolaj’s parents that the tumour was diffuse, meaning that it had spread, and for the first time he suggested that he may not be able to remove it all.
Although the Barmans were alarmed at this last-minute news, they felt it was too late to back out.
After a 10-hour operation, Teo spent 10 minutes telling the parents that he’d removed 85 per cent and that it appeared to be benign. With that, Teo was gone, and they never saw him again.
However, after the operation the pathology results revealed that the tumour was not benign. It had the “H3K27M mutation”, which is the defining molecular marker for the devastating DIPG.
According to Souweidane, if a biopsy comes back “consistent with an H3K27M mutation, my opinion, and I think the consensus of most neuro-oncology individuals, is going to be not to resect, not to offer surgical therapy.”
Before surgery, if Teo doubted the two previous diagnoses of a DIPG, he could have done a biopsy to be certain. But he didn’t, and rather than delivering a miracle, Teo left the Barmans with a nightmare. Their once happy and playful little boy would never walk, talk, or eat on his own again.
With the medical costs piling up in Singapore, the Barmans had to pay $40,000 to hire an air ambulance to fly Mikolaj back to India, where he languished in intensive care for months. Mikolaj’s care cost nearly $250,000 and the rest of his short life was spent in a room staring at a ceiling, his only means of communication was blinking his eyes.
There was no hope. For a DIPG, there is no hope. So why give the false hope in the first place?
Prasanta Barman
Ten months after the catastrophic operation, the inevitable happened: the aggressive tumour returned and Mikolaj died.
Mikolaj’s MRI scans were shown to several neurosurgeons who immediately identified the tumour as a DIPG. When told that an unnamed surgeon, offering a cure, had performed a resection, they were horrified.
Barman is racked by guilt at what he put his son through. “There was no hope. For a DIPG, there is no hope. So why give the false hope in the first place?” he asked.
Bella’s battle
Mikolaj Barman was not the only one. A year after Mikolaj’s death, another family was facing the dire diagnosis of a DIPG.
In April 2020, doctors at John Hunter Hospital in Newcastle told Gene Howard and Sarah Higginbottom that their seven-year-old daughter, Bella, had a DIPG and that there was nothing that could be done except to provide radiation as part of palliative care.

Gene and Sarah Howard with their daughter Bella.Credit:
Howard refused to accept that there was no cure and, in desperation, he turned to the high-profile Charlie Teo.
Teo’s notes after the initial consultation reveal that he “agreed that this is likely to be a DIPG”.
Bella’s grandmother Mariza Howard, who was at the consultation, recalled Teo telling them there was a tiny chance the scan might be wrong. Teo offered to do a biopsy and, while doing that, if there were parts of the tumour he thought he could remove to buy Bella more time, he would.
I was just a little perplexed how an operation that could save someone’s life [was] contingent on a payment of money the very next day.
Mark Ramsland, a Howard family friend
“At this point we were all in tears because … there was no hope and then we got this possibility of hope, a doctor … out there offering something,” recalled Gene, a tradesman from Shoal Bay.
Instead of waiting for conclusive biopsy results, Teo wanted to operate the very next day. The Howards leapt at the chance to extend Bella’s life. However, there was a catch. The surgery would cost $100,000 and $50,000 had to be in Teo’s bank account that night.
“We were trying to figure out how to get it ourselves, but even to get a loan it takes weeks, even friends that have lots of equity – for them to get a loan it takes weeks,” said Gene who, in desperation, even tried to sell his kidney.
“I wasn’t ever stopping until we got that money,” he said.

Sarah and Gene Howard in the bedroom of their daughter Bella who died of DIPG.Credit: Peter Stoop
Mark Ramsland, a friend of the Howard family and their solicitor and cancer survivor himself, was troubled at the haste for the surgery, the absence of an oncologist, and the extraordinary amount of money that had to be in Teo’s account that night.
“I was just a little perplexed at how an operation that could save someone’s life needed to be contingent on a payment of money the very next day,” the solicitor said.
Gene’s boss loaned him the money and the operation occurred at Prince of Wales Private Hospital in Sydney the next day.
Just how much of the tumour Teo removed would vary. Immediately after the surgery, Gene Howard was ecstatic when told by Teo he’d removed 95 per cent of the tumour which, in his opinion, was low-grade and slow growing.
The operation report recorded a greater than 50 per cent resection and, in a report dated June 2, 2020, Teo wrote that “naysayers” would say he hadn’t removed any.
Experts in this area told the joint investigation that even if 99.9 per cent of the tumour was resected, which would likely result in immediate death, a resection is pointless as the cancer has already spread and it will come roaring back.
The cancer cells “are going to continue to grow”, Kieran said. “They basically are going to take over the entire brain because they don’t respond to surgery, they don’t respond to radiation, and they don’t respond to any currently known chemotherapy. Unfortunately, we do not cure kids with DIPG.”
Three days after the operation, the pathology results came back. Bella’s tumour had the H3K27M mutation and the diagnosis was a DIPG. But in his report, Teo cast doubt on the validity of the H3K27M mutation as an indicator.
While radiation is the accepted treatment to relieve the symptoms, Teo advised against this.
In his report, he noted that he had counselled the Howards that “many neuro-oncologists and reputable neurosurgeons would be aghast at this course and would be strongly recommending radiotherapy plus or minus chemotherapy” but that Jean [sic] “is fully aware of the two completely different options” and that it was his choice not to have the radiation.
Teo offered the Howards a second operation at the same price as the first, but as the Howards were driving back to Shoal Bay after Bella’s 12-week scan, Teo rang with some shattering news. He told Gene to pull over and get out of the car.
“Mate, this is really bad. The scan’s come back, it’s grown ... probably three times as big as what it originally was,” Teo told him. Sarah said she cried the entire way home.
Bella deteriorated quickly and required 24-hour care. In January 2021, eight months after diagnosis, Bella died surrounded by her devastated family.
Her official cause of death was recorded as a Diffuse Intrinsic Pontine Glioma.
In a written response to questions put to Teo about his DIPG operations, a spokesman said: “Diffuse Intrinsic Pontine Glioma (DIPG) /Diffuse Midline Glioma (DMG) is the most aggressive childhood brain cancer. It is incurable and is truly inoperable. Dr Charlie Teo has never operated on a pure DIPG/DMG, and has never recommended surgery on such a tumour.”
While Teo declined a request for an interview with the joint investigation, he told The Daily Telegraph on Saturday that the debate around “inoperable” brain stem tumours was a complicated one and “misinformation was rife, even among neurosurgeons in Australia and around the world”.
The article also stated, “Virtually every intrinsic primary brainstem tumour is labelled as DIPG because ‘there is no real definition and no one wants to talk or think about having to operate on them’, he said.”
“That’s why all these authorities are saying Teo is operating when he shouldn’t. No, they have got it all wrong,” Teo told the Telegraph.
In August 2021, seven months after Bella Howard died, the NSW Medical Council was so concerned about Teo’s operations on brain stem tumours, including a DIPG, that they placed restrictions on his practising certificate.
In November 2021, Healthscope, which runs 41 private hospitals, withdrew Teo’s accreditation at Prince of Wales Private Hospital, where he has worked for years.
In September, Teo was due to face a two-day disciplinary hearing after a lengthy investigation by the Health Care Complaints Commission. However, it was postponed to a date to be fixed as one of the hearing days became a public holiday due to the death of the Queen.
Rather die than go blind
Joe Leslie, a Brisbane engineer, discovered he had a slow-growing brain tumour in 1996.
After several operations over the years, in 2018 doctors told him that there was nothing more they could do to treat his brain tumour and estimated he had two years to live.
Having heard of the renowned brain surgeon, Joe and his wife, Kathy, a nurse, sought a second opinion.
At the consultation, Teo assured the Leslies that he could remove the tumour. He dismissed concerns raised by the Queensland doctors that because of the position of the tumour, any attempt to remove it would leave him blind.
Kathy Leslie said Teo told them not to worry, it was unlikely that that would happen as he’d been doing these surgeries “for ages” and he was “way better” than other surgeons.
She recalled Teo saying: “the other surgeons were jealous of him because what he could achieve and … he was a lot better than what they were saying and he could achieve great things”.
For Joe, the one thing he impressed upon Teo was that he didn’t want to go blind. “He would rather have passed away than go blind, that was his big thing,” his wife said.
Kathy recalled being anxious about the decision to proceed. “It wasn’t my life. It was Joe’s decision because it was his life, but my gut feeling was telling me maybe we should just go off and … enjoy what we’ve got.”
Teo assured them Joe would be back at work in no time.
Having paid Teo $35,000 from their retirement savings, Joe’s surgery was scheduled to start at 3pm. Due to complications with a previous operation, his surgery didn’t start until 9pm and didn’t finish until 5am the next day.
Kathy was worried about the surgery starting so late at night. She told the joint investigation she was told Teo had to fly to Singapore the next day, so it had to be done then. “What was so important that he had to get on that plane and go, rather than giving quality of care?” she posed.
Following the surgery, Joe was blind. And what Kathy Leslie couldn’t have known was that Teo was jetting off to Singapore to operate unsuccessfully on another patient, four-year-old Mikolaj Barman.
There were serious post-operative complications, including cerebrospinal fluid (CSF) leaking out of his nose. Joe spent six weeks in and out of hospital in Sydney before returning to Brisbane, where he spent months in a public hospital.
Joe Leslie lost more than his eyesight. The 65-year-old is brain-damaged, confused and requires 24-hour care. He didn’t have the capacity to provide consent to be interviewed.
“The life he lives now, the old Joe, the Joe that we knew, would be horrified what his life has come to,” his wife said.
Kathy Leslie, who has had to go back to work to support the family, is angry at what she believes is the false hope Teo gave them.
“Doctors take an oath of ‘Do no harm’. This has done more harm than good: emotionally, physically and mentally. The strain you put on families when you do operations like this is a lot more than if you would lose someone.
“Yes, you did the operation. Yes, you took the tumour, but what quality of life did you leave him with?” Kathy said.
She wanted to know if Teo would want to live the nightmare that Joe is living. “That’s what I would like him to say … Is the quality of life you want for yourself? Why do you do it to other people then?″
Do you know more? Email: kmcclymont@smh.com.au
The Morning Edition newsletter is our guide to the day’s most important and interesting stories, analysis and insights. Sign up here.