AS the hot sun beats down on the red dirt of Bathurst Island, three-year-old Joel Heenan sits inside a renovated shipping container outside the community’s health clinic.
The steel rectangle been transformed into an audiology booth, allowing young Tiwi Islanders to get their ears tested by specialists.
Clutched in Joel’s tiny hands is a picture book with bright illustrations of dogs, babies and sheep. He slowly flips through the pages from the warm comfort of his uncle’s lap.
From behind a closed door a button is pressed and a warbling high-pitched sound fills the room.
Joel doesn’t hear it. He’s distracted, fiddly. The sound continues to ring. He still isn’t sure.
Finally, he looks up — and is treated with the sight of a bouncing toy as a reward. A cheeky grin from Joel but the test is no laughing matter.
The fact is at only three-years-old, little Joel already has moderate hearing loss.

■ ■ ■
JOEL’S mum, Rowena Tipiloura has four kids. Two of them have problems with their ears.
Joel has a hole in his right eardrum, something which may soon need an operation. Joel’s big sister had an operation to patch up a burst eardrum when she was only six.
“After the patch, it’s been much better,” Rowena says of her older child.
“Joel is not too bad, he talks a lot at home. Knows his fruit, animals, loves his uncles.
“They got a little problem.”
Rowena’s not worried about her youngest child’s hearing, believing it is good enough to get by.
It’s not neglect, not disinterest, not out of a lack of compassion for Joel.
Rowena clearly loves her son — it’s obvious in the tender way she holds him, the way she strokes his short, fluffy hair and the way she lights up when she talks about his love of family. Rowena wants the best for Joel.
But his ears just aren’t her biggest concern. Not when it’s so normal for people to be hard of hearing in her community. Not where there are so many other significant health concerns to worry about.
■ ■ ■
JOEL is one of 425 Australian kids under the age of three taking part in an ear health study with the Menzies School of Health Research.

The program has been running for nearly seven years and, so far, the findings paint a disturbing picture about the ear health of kids living in remote Territory communities.
One toddler in the study has had an active infection and burst eardrum for six months. He’s only 18-months-old.
And in another case, an ear infection was recently detected in a four-week old baby.
Aboriginal kids have the highest rates of otitis media, a middle ear infection which can cause hearing loss, in the world.
According to federal health figures, only five per cent of one-year-old indigenous kids living in remote communities have bilateral normal hearing. This means 95 per cent of one-year-old indigenous kids living in remote communities can’t hear normally out of one or both of their ears.
Last year, thousands of hearing specialists services were provided to Aboriginal children and other young people in the NT.
But still, nine in 10 Aboriginal kids under the age of three in remote Territory communities have ear disease. Most of them will develop hearing loss which will affect their early brain development and set them on a path of disadvantage.
Early diagnosis and treatment in the first 1000 days of a child’s life can treat the disease but that rarely happens.
Disturbingly, just 13 per cent of the 2000 cases Menzies researchers recently examined and prescribed antibiotics for were followed up using best practice.
Which means just 13 per cent of the kids in desperate need of treatment are getting what they need.
■ ■ ■
EARLY next year, the $7.9 million Hearing for Learning program will be rolled out across remote communities in the NT.
The five-year initiative aims to address chronic hearing problems in Territory kids and is jointly funded by the NT Government, Federal Government and the Balnaves Foundation.
It’s expected to reach 5000 Territory children, with a focus on kids under three.
Infections are hard to pick up in babies because they rarely show signs of being in pain, which is why frequent checks are vital.

Led by Australia’s first indigenous surgeon — ear, nose and throat specialist Dr Kelvin Kong and Menzies School of Health Research professor Amanda Leach — the program will train and employ community members to help diagnose and treat ear disease and hearing problems in local children.
But how can this program work when so many before it have failed?
Prof Leach is realistic about the challenges facing service delivery in remote areas and is concerned at how many people fail to follow up with treatment.
“The guidelines say the children (prescribed antibiotics) should be seen within a week to make sure the ears aren’t getting worse, but that isn’t happening,” she says.
Prof Leach says ear disease is so common in remote Territory communities, it’s “normal” for young kids to struggle to hear.
Sadly, this “normalising” of the condition means parents don’t worry when their children show signs of hearing loss or “pus” ears.
In remote communities, Prof Leach says indigenous families face so many immediate health concerns — like rheumatic heart disease, hunger, housing instability — that issues with hearing quickly falls down the priorities list.

“Ear disease to a large extent is poorly understood and underestimated as a health issue in remote communities, they are dealing with a lot of other things,” Prof Leach says.
“The resources to deal with this issue are totally inadequate.
“It’s just overwhelmed with other issues in the clinic, and I think the families are probably very busy with things as well.”
Many people living remote don’t have reliable cars to travel to a health clinic, and as it’s not a service which can be delivered in homes, explains Prof Leach.
Even if they get to the clinic, ear specialists only visit remote communities every few months so the responsibility for checking ears falls to clinic staff.
And staff are often overwhelmed with other checks or not properly trained to use specialist equipment.
Even if they do remember, ear tests aren’t always pleasant — and a wiggly, irritated, and crying child rarely provides clear ear test results.
But Prof Leach is optimistic this new program can succeed where others have failed.
She says chronic ear conditions in remote communities won’t be cured by flying in more specialists but by upskilling community members who have strong connections with local families.
“The question is — how can we bolster resources within the community so there’s an expert within the community every day — so there is someone there to look at these kid’s ears, do those follow ups, support the family and support the fly in-fly out services that are still needed,” she says.
After a six-month training program, trained locals will act like the “glue” between primary healthcare providers, fly-in, fly-out specialists, families and the kids.
These workers might not have a medical degree but they have an established relationship with families and can note down red flags for follow-ups.
“If we do this well, it should work, and it should be a good model for communities to take more — more control of the country child healthcare — it’ll better inform the community, the family, the children, themselves,” she says.
■ ■ ■
MENZIES research nurse Beth Arrowsmith has been studying the ears of remote Territory kids for about five years.
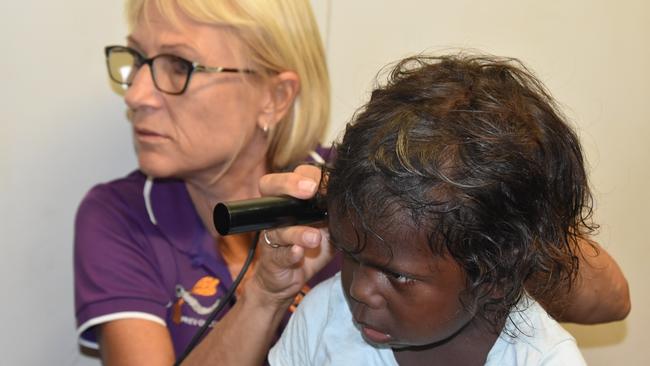
In all that time, she’s seen no “real improvements” in the rates of ear infections.
Ms Arrowsmith says until remote indigenous Australians are no longer living in poverty, ear infections will continue to plague them.
“We put it down to the social determinants of health, it’s overcrowding, its poor hygiene, its nutrition, the availability of services, specialists — all of those things combined,” she says.
“You’re talking about ear disease, it’s not a new thing. Any headway is very slow to make.
“It will be a very long time — the housing is inefficient, there is overcrowding. We spoke to a mum the other day who had 18 people in their house. 10 kids and eight adults.
“How can you possibly keep clean in that environment?”
Audiologist Janine Pisula says ear disease in indigenous communities isn’t a new issue, but it is a serious one.
“We’ve got to remember that the community brings up a child,” she says.
“And the community is so used to people with ear disease that they automatically do things to accommodate them.”
Ms Pisula wants the focus put back on ears — as hearing loss can impact a child’s potential.
“Kids with better hearing speak better, more clearly — they find it easier to learn, to understand the world around them,” she says.
“Hearing loss can impact someone for their whole life.”
Young kids with hearing loss are more likely to fall behind in school, become disconnected from their peers, and struggle to build relationships as they grow older.
And older people with hearing problems are more likely to feel depressed and develop dementia.
■ ■ ■
MURRUPURTIYANUWU Catholic School on Bathurst Island welcomes kids from preschool to year 13.
For nearly all of the students enrolled at the community school, English is not their first language — with the majority of indigenous kids speaking Tiwi at home with their families.
Deputy principal Stacey Marsh says hearing problems are a “huge” issue at the small school, but the kids themselves aren’t keen to wear aids that make them stand out.
“We don’t know if it’s the language barrier or the ears,” she says.
“When children can’t hear you, they can’t learn. It’s very hard to get the message across.”
Teacher Caroline Bourke has been at the Bathurst Island school for about three years and is worried about the long-term opportunities for kids on the island.
Of the indigenous population behind bars in the NT, 90 per cent have hearing loss.
It’s a troubling statistic which shows a clear downward spiral.
“(Poor) hearing is an enormous problem, it impacts big time on what they’re able to take home from lessons,” Ms Bourke says. “It’d have to be the biggest problem we face.”
She estimates 60 per cent of the kids at the school have trouble hearing, but says any new program set up to tackle the issue will have to go to the families — instead of expecting families to travel into the clinic.
One solution she sees is hearing tests and treatment options rolled out at school, which should improve the treatment rates of young kids.
■ ■ ■
IN the metal audiology booth, little James Orsto, 3, rolls a blue plastic truck along the table in front of him.
His mum, Gregorianna Orsto, watches her boy’s slow calculated movements from a chair just an arm’s length away.

From the other side of the screen, Janine Pisula presses a button and the same high-pitched warbling tune which alluded Joel echoes across the tiny room.
Instantly, James stops, and points at where he knows a toy is about to jump around.
Straight away, the tiny Tiwi Islander is greeted with the sight of a bouncing teddy.
He grins, and quickly returns to the toy truck in front of him.
Gregorianna smiles at her boy. James is her youngest son and his hearing is a priority.
“It’s very important,” says Gregorianna.
“(James) has no problems with his ears, he’s chatty at home.
“He’s really helpful at home, he can say ‘Mummy’, ‘Daddy’, ‘tea’ — he loves drinking tea.”
Gregorianna’s older boy, Angelo, had problems with “pus ears” when he young, so she knows the warning signs of ear disease.
Her partner’s ears sometimes cause him pain, and his hearing is far from perfect.
She doesn’t want little James to have the same challenge, so when specialists visit Bathurst Island in a few shorts months, Gregorianna will make sure her youngest son has his ears checked.
She’ll do everything she can to make sure James’s future sounds bright.

Add your comment to this story
To join the conversation, please log in. Don't have an account? Register
Join the conversation, you are commenting as Logout
‘I have fallen in love with the NT’: Story of a Ugandan-born lawyer
This Ugandan-born lawyer has overcome a lifetime of obstacles to finally get admitted to law in the Northern Territory. Read his story.
‘Treated like animals’: Death in custody warning over watch house
Women are allegedly being crowded into cells in view of masturbating men at the Territory’s police watch house. WARNING: Distressing images.