Tom Wallis, Northern Beaches Hospital: Doctor reveals what it was like on the COVID-19 frontline
They are the heroes of the moment. The medical staff on the COVID-19 frontline. Here’s one doctor’s story.
Manly
Don't miss out on the headlines from Manly. Followed categories will be added to My News.
- The Night Watch documentary series launches
- ‘We could taste fuel’: How river rescue went horribly wrong
- Bang, then smoke: How family escaped Sydney house explosion
Intubating a COVID-19 patient is when they’re at their highest risk of dying – and for the health workers trying to keep them alive it is when they’re most likely to catch the virus.
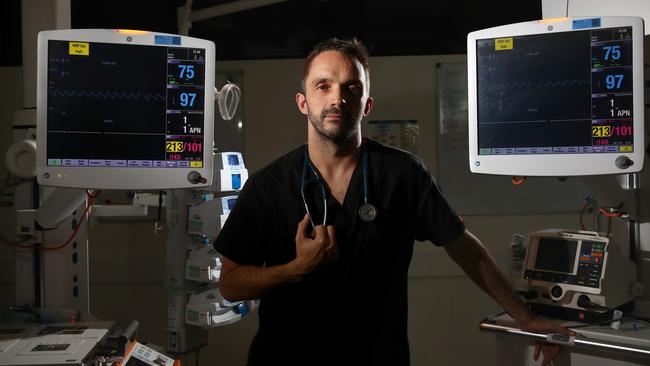
Dr Tom Wallis, who has led the Emergency Department’s COVID-19 response at Northern Beaches Hospital, worked 90 hours weeks often into the night preparing for the peak of the pandemic.
One of the most important roles for the core team was practising intubating a fake patient over and over.

Even so, when they had to do it for real patients, it was anxiety inducing.
“In that environment we are all pushed to the edge of our comfort zone,” he said.
“You are very much aware of your own vulnerability.
“It’s also a high risk procedure where patients are at risk of passing away.
“We know this person is someone’s father, mother, brother or sister.
“The patient is also scared, they know they have this strange virus.”

Dr Wallis, 39, of Manly, said this was the moment the team need to be wearing the highest level of protection, which includes respirators, similar to the bottom half of a gas mask, to limit the risk of contracting the virus.
Apart from intubation, there are various zones during a pandemic and the “hot zone” is where staff are caring for a coronavirus patient and are required to wear masks rather than respirators, as well as the full personal protective uniform of goggles, gown, gloves, surgical nets in some cases, and hospital socks.

“The PPE is uncomfortable, you get pressure sores on your nose, very sweaty and dehydrated but you can’t have a drink of water or a coffee without leaving the zone and taking everything off,” Dr Wallis said.
“There’s no touching your face and just constantly being aware of not doing that is tiring.
“For that reason, staff are only in the hot zone for a maximum of four hours otherwise that’s when mistakes start to happen.”
Dr Wallis, born in the UK, said seeing hospitals overseas being overwhelmed with patients was worrying.
“There was a sense of impending doom and wondering how it would all unfold,” Dr Wallis said.
“It was frightening watching colleagues (abroad) getting very sick or sadly passing away.”

He said the government’s response and the community’s support of social distancing was outstanding and helped avoid a similar fate here.
He said the experience had brought colleagues together, cemented relationships and improved communication with GPs in the community.
He said the hospital was no longer on high alert, but no-one knows whether they will be a second wave.
“This virus isn’t going anywhere,” he said. “We will have to open the borders eventually.
“But if it does happen we have had time to rehearse things.”

