Mysterious ‘missed call’ exposes ‘harrowing’ Aussie bush problem
A mysterious ‘missed call’ has exposed a Aussie bush problem that nearly cost one NSW woman her life and is leaving others traumatised.
Real Life
Don't miss out on the headlines from Real Life. Followed categories will be added to My News.
A mysterious ‘missed call’ has exposed a Aussie bush problem that nearly cost one NSW woman her life and is leaving others traumatised.
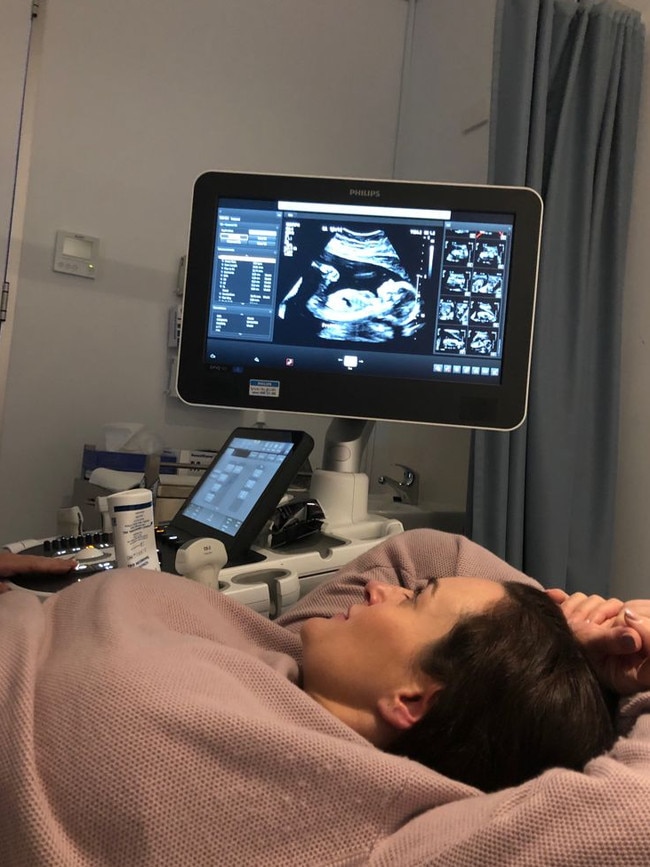
Leah was 8 weeks pregnant when she travelled from her Narrabri hometown in central New South Wales to Tamworth for a routine ultrasound in April 2020.
Heartbreakingly, she was told the pregnancy wasn’t viable and she would need to have a D&C, a common procedure to remove tissue from inside the uterus after a miscarriage or abortion.
Leah and her husband Pat remained in Tamworth, two hours away from their home, and she had the procedure the following day, before travelling home the day after that.
One week later, Leah’s obstetrician called her and asked her to get a blood test, as no foetal matter was detected following the D&C. Leah noted the doctor seemed very calm and unconcerned over the phone, so she wasn’t worried and followed her doctor’s instructions and had the blood test.
Two days later, Leah missed a call from a private number, however no voice message was left. This mysterious call would determine Leah’s near-death experience.
Post-procedure complications
That night, the Narrabri local began to feel unwell and thought she may be coming down with the flu or gastro. She woke in the early hours of the morning in excruciating pain. She got out of bed, fell to the ground and blacked out. When she woke up, she called out for her husband, saying she couldn’t breathe properly. She started vomiting and fell unconscious again.
“I remember needing to vomit and getting out of bed, feeling a huge stabbing pain. I woke up on the floor of the bathroom feeling sick, dizzy, vomiting and really struggling to call out loudly to Pat in the bedroom,” Leah recounted to news.com.au.
“I was confused at feeling so terrible and unable to get off the ground because when I went to bed I thought it was just food poisoning.”
Leah’s husband also said he assumed at this stage that his wife just had a stomach bug, but when she became unconscious he quickly called the ambulance.
Over the phone, Pat told ambulance officers that Leah had a D&C a week prior, but had no more information other than that.
“I was probably more confused than scared at that stage,” he said, admitting that first triple-0 call he made was fairly “sobering”.
Rushed to hospital
Leah was taken to Narrabri hospital where an ultrasound was performed, which showed a foetus and significant blood pooling. The couple were beside themselves as the on-call doctor kept telling them they could see a foetus.
But how was that possible, given she’d had a D&C a week ago?
“I’d been given pain meds by that point, I remember thinking, ‘there’s no baby, I had a D&C, there’s no baby, stop telling me there’s a baby!’ But whether I actually said anything to the doctor, I don’t know,” she said.
It was later determined that the missed phone call from a private number was Leah’s obstetrician, calling with her blood results which indicated that she had in fact had an ectopic pregnancy and the unviable foetus had not been removed a week prior.
“It took a fair bit to sink in,” Pat said. “Obviously the D&C was fairly harrowing in its own right and it had never occurred to me that it mightn’t have retrieved everything. So at that point I was starting to panic. But more so the internal bleeding was an issue right from the outset. There was a big black mass and it was getting bigger.”
With Leah’s life at risk, Narrabri Hospital had no surgeon on duty, nor did the hospital have one on call. Staff on duty requested for a chopper transfer but due to Covid-19 and what Leah claims were rostering issues, the helicopter was on stand-down and so unable to transfer her to Tamworth, two hours away by car, or to John Hunter Hospital in Newcastle, just shy of five hours away, for lifesaving surgery.
Leah’s husband vividly remembers the doctor telling the paramedics that they must take her to Tamworth, however paramedics said it was too risky because her blood pressure was too low and if it went any lower they didn’t have the specialist equipment to deal with it.
The doctor then said “she will die here, take her and give her the best chance to make it”, so the decision was made to make the journey by ambulance.

The ambulance ride
The ambulance made it to Tamworth hospital in 45 minutes, with Pat travelling behind in his car, unsure if his wife was alive or dead.
“That’s the hardest thing I’ve ever done in my life other than sitting outside the waiting room at Tamworth,” Pat recalled of that solo two-hour drive, unable to keep up with the ambulance ahead.
“I was hoping the whole way that the phone wouldn’t ring. I hadn’t told our family anything and it was 5am on Monday morning. I knew I couldn’t hold a conversation without breaking down so I tried to draft a text in my mind to our parents.”
Pat said he had to pull over briefly and “cry in the toilets halfway” due to the sheer gravity of the situation.
“I hadn’t slept or eaten and I was just in a daze and emotionally buckled.”
Similarly, Leah said the ambulance ride “was the most traumatic part of the whole experience for me and something that I’m sure will stick with me forever”.
The terrified Narrabri woman, who was on heavy pain medication at this point but still in agonising pain, said the paramedics were amazing on the journey and recalled them giving her a blood transfusion towards the end of the trip.
“It was only on arrival at the hospital where they wheeled me into a room with so many medical staff gloved up ready to go that I realised that this was really bad,” she said.
In the Emergency Room
With Pat still making his way to the hospital by car, Leah called her husband from the gurney as she was being wheeled into the operating theatre.
“When the phone rang I was in pieces because the bloke wheeling her in wouldn’t tell me anything other than ‘she’s about to be operated on and I think you should take the chance to talk to her’,” he recalled.
“I knew what that phone call was but you can’t say goodbye and I didn’t want her to be even half as scared as I was.”
Thankfully, Leah’s emergency surgery was a success. She lost a fallopian tube and spent six days recovering in hospital. One of the most challenging parts of the whole experience was being placed in the maternity road during her recovery “when struggling with fertility issues and no baby, re-mourning the idea of who that foetus could have been … wondering if I could have a baby with only one tube”.
Leah said every nurse or doctor who came in to see her during those days in hospital would read her file and say “do you know how lucky you are to be here?”
“Recovery once home was physically painful and as you’d expect a very emotional time,” she said.

Starting their family
Leah ultimately changed obstetricians after her near-death experience. To this day, she believes had she connected with the doctor on that fateful phone call to learn of her ectopic pregnancy, she would have immediately travelled back to Tamworth to be seen by specialists, and would not have put her life at risk by continuing on with her weekend as normal.
Watching his wife nearly die, Pat also suffered significant trauma and admits the journey to eventually become parents was an extremely difficult one, mentally.
The couple are now parents to three daughters, Maisie (3.5 years old) who was born via IVF, and twin girls, who are nearly 2.
“The twins were pure chance natural conception and so close behind [our first daughter] that you kind of just had to laugh,” he said.
“It was hard the whole way though, just thinking that if there were any complications its basically a dice roll on whether you’ll get to the required facilities in time.
“It’s a different sort of fear when you’ve got a kid cause you’re more concerned for them and that they could lose their mother than you losing your wife.
“To be frank, if Leah had decided she couldn’t go for kids I wouldn’t have paid it a second thought or batted an eyelid, but I also fully understood that she didn’t want a near miss to define such a big part of her life.”
A spokesperson for Hunter New England Local Health District said: “Maternity services in NSW are networked, ensuring women and their babies receive the safest care at the most appropriate facility. From the outset, women, their support person/people, and our dedicated maternity staff work together to plan for the birth and ongoing care.
“The woman’s birth plan is constantly reviewed and updated with the woman, throughout her
pregnancy, ensuring that recommendations and decisions are always made in the best interest of both the woman and her baby,” the spokesperson told news.com.au.
However, sometimes these plans change – whether due to the need for specialist care, unexpected workforce shortages, or other unforeseen circumstances.
When this happens, we acknowledge how disruptive it can be, especially if the location of the birth needs to change, and we sincerely apologise to any women who have experienced this.
“While we’re unable to comment on specific cases due to privacy, we acknowledge the distress these women have experienced.”

The Bush Babies Campaign
Leah and Pat are sharing their story as part of the Bush Babies Campaign, which is advocating to address critical issues in maternity care in rural, regional and remote areas.
“We urge the Government to allocate bundled funding across all maternity settings and care providers to promote equity in funding and service delivery, ensuring all women have access to quality maternity care, regardless of location,” is one such demand.
Leah and Pat believe the centralised care model for New England and North West residents – all routed through Tamworth – is putting enormous pressure on an eroding system and mistakes are being made. The sheer geographical distance between hospitals means centralised care is simply not working.
“At the end of the day you either need more services locally or stronger pathways to those services, ie more doctors or more choppers. The doctors solution is as old as time. But how do you get more professional specialists out to rural areas?” Pat said.
More Coverage
Originally published as Mysterious ‘missed call’ exposes ‘harrowing’ Aussie bush problem





